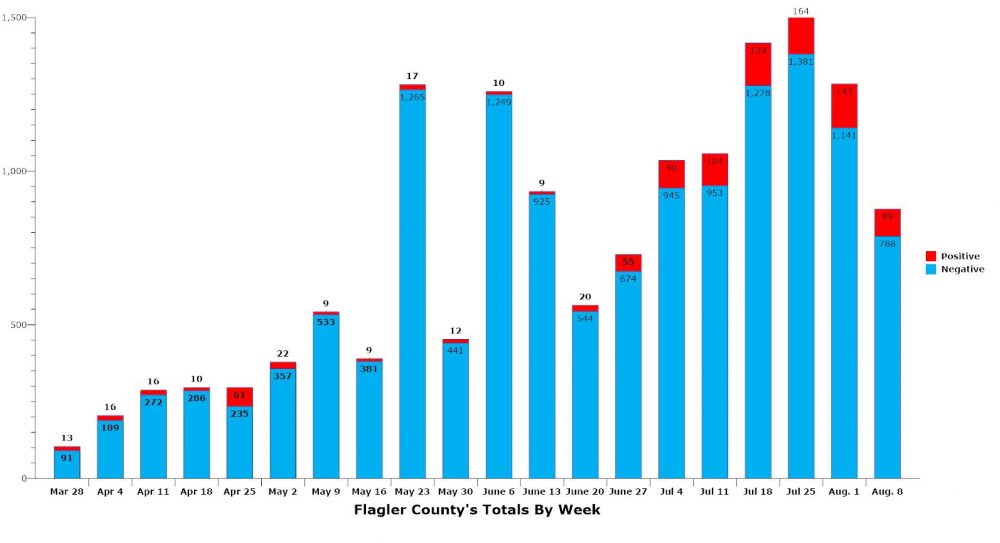
The Florida Health Department today reported that with the addition of 19 new cases in one day, Flagler County crossed past the 1,000-case mark–“a little milestone,” as Flagler Health Department Chief Bob Snyder described it. Thirteen local residents have died since the pandemic began to spread in the county. While numbers are stabilizing, they are doing so at still much high numbers relative to the April wave.
In the first six days of the current week Flagler has tallied 89 new cases–a lower number, relative to the the three previous weeks, but testing has fallen off too, with a total of 877 tests confirmed by the state health department in the first six days of the week, and a positivity rate of 10.1 percent–at least according to the state. Snyder continues to report a different, lower rate that includes multiple negative tests for the same individuals, which artificially lowers the actual positivity rate.
Among those confirmed positive in Flagler in the last 48 hours are a 4-year-old girl and a 17-year-old boy, but all others were adult, and the median age in the last two days was just over 50.
But the trends are downward–in lower confirmed cases, lower local hospitalization, and fewer people going to the hospital with covid-like symptoms, though the number of people going to the hospital with influenza-like symptoms has been rising since early July. As of this afternoon, 15 people were hospitalized at AdventHealth Palm Coast with a primary diagnosis of covid-19, according to the Agency for Health Care Administration.
“It’s been like that for the past week or so. So it did decrease, but for the past few days it just stayed around that same number,” Wally de Aquino, the hospital’s chief operations officer, said this morning during WNZF’s weekly covid wrap-up.
There have been no new confirmation of cases at local assisted living or group home facilities since the beginning of the week.
The trends are being eyed by school officials, with a scheduled reopening on Aug. 24, two weeks later than originally planned. The district has’t explicitly stated what positivity rate–or what other criteria–should be a threshold, but the local health department, echoing the World Health Organization, has generally set a 5 percent positivity rate as a threshold below which certain gatherings, including schools, may resume, assuming strict guidelines are followed. Only 63 percent of students are expected to attend class in person, at last count, and will be required to wear masks in grades 3 and up while observing social distancing rules.
“It’s obviously a team approach and we do want to pay attention to our local conditions, and that’s why it’s critically important that DOH and Bob Snyder is involved,” Cathy Mittelstadt said this morning, summing up the strategy as managing risk. “I have a safety specialist who takes care of following those guidelines as they might change from the CDC, and then all of our district directors work with that safety specialist to make sure we’re setting up the stage for everybody to be in a great situation when we bring our teachers and students back.”
All sports seasons have been suspended until further notice. Academically, the district is offering three options for students, two of them virtual, enabling students to stay home.
Snyder, however, has made it clear: “I prefer the virtual learning,” he said. “Keep in mind I’m Health Officer Bob and of course I want kids to go back to school, but I’m just pleased to see two of the three options were virtual learning, because it’s going to make it easier for us to social distance the remaining children in school.” He said he was comfortable with the 60-odd percent of students who would attend, “and so glad there’s options for parents.”
According to the latest report on children and covid in Flagler and Florida, the number of children in Flagler who are contracting the virus continues to grow, with a cumulative 79 testing positive out of 683 tested, and a cumulative positivity rate of 11.6 percent. But the overwhelming majority of those positives have been since July 1, with a higher positivity rate.
Flagler’s numbers look better only when set against the state’s, which has seen 40,400 children test positive and a positivity rate of 15 percent. As of today, 436 children have been hospitalized, seven have died, the youngest a 9-year-old Putnam County girl. Four of the deaths are in the 15 to 17 age range.
Testing delays continue to be a problem. “I got a call from a couple who had their test at Daytona State, it was sent to Quest lab, it was July 21, and still did not get a test result back as of yesterday,” Snyder said, “so I had my team look for it. Still it had not come back. It’s just a shame, because so many days pass, but thank God we are using a new lab called MDL.” The test results from that lab are returning in two to five days, according to the health department.
The pandemic is having an effect on voting: early voting for the Aug. 18 primary began on Monday in Flagler. “So far we have 1,800. That’s it,” Elections Supervisor Kaiti Lenhart said of the early-voter tally to date. “It’s about half of what we should have right now, comparatively.” That’s compared to 2018. Lenhart said it was due to people’s fears of the virus. On the other hand, her office sent out 29,000 vote-by-mail ballots. But that doesn’t mean the ballots will all be sent in. “We have to have it–received in the office on Election Day by 7 p.m.” The postmark does not extend the deadline.
Florida passed the half-million mark in cases earlier this week after adding nearly 50,000 cases in the last seven days. Only California has had more cases in the nation (541,000), though Texas is closely behind Florida, with 488,000. Deaths in Florida continue to accumulate rapidly, with over 1,200 in the last seven days, for a total of 8,051.
De Aquino shed new light on the shuffling of patients that takes place between local hospitals in the same network. When there were situations to where we felt that we as an organization felt that a particular hospital was getting closer to its capacity,” he said, “then we would reach out to another hospital to see if there was capacity so we can send patients that were actually in the emergency room, that were actually scheduled to be admitted. So we wouldn’t take a patient that’s already in the hospital to move them. We actually have a call every day around 12:30 to do an assessment across the region, to make sure that we can leverage each other in terms of capacity.”
Similarly, AdventHealth Palm Coast was in a position to care for patients from counties that were nearing capacity, Volusia especially. “We did help a few other hospitals I would say three weeks ago, four weeks ago,” de Aquino said.
Treatment has evolved, and one of the ways the hospital is handling certain patients who don’t need hospitalization but still need to be monitored is to send them home, tethered to a system called Vivify, a private company that enables remote monitoring of patients.
“The problem with the patients that we see who come in who are a little sick, we do a test, they’re not ill enough to be hospitalized,” says Paul Mucciolo, who heads AdventHealth Palm Coast’s emergency room and who appeared alongside de Aquino on this morning’s covid update. “They certainly don’t need that level of service. But the Vivify allows us to keep an eye on them at home. What it does is set them up with a system for outpatient monitoring. Their oxygenation, they have physician follow-ups, virtually, they have access to a nurse line, information line, etcetera, etcetera, etcetera. What that does is give people a great security blanket at home. Importantly the number of patients who we test who have symptoms, who go home, the numbers that have to come back to get hospitalized is in the low single digits. I can’t emphasize that enough. Most people do well at home.”
Mucciolo immediate advice: “Don’t get your guard down. The important thing is people have to continue to wear their masks. They have to wash their hands. Eye protection is important, and to wear your mask properly. Make sure it covers your nose, make sure the loops are on your ears and it’s down over your chin. I can’t tell you the number of people I see who come in the department, the staff instructs them on how to put on the mask correctly, they make sure it’s a correct fit. They come in or a visitor comes in and I walk in the room and the mask is hanging off their chin, or hanging below their nose. We have to do that–we have to wear them properly.”
But the ER chief said people are still shying away from the ER out of fear that they would contract covid–thus potentially aggravating what conditions they may be suffering, from infected wounds to stroke patients who have had symptoms for five days.
![]()

























Kathy says
Well, doesn’t less testing mean there are less people getting sick. I hope so. 🙏❤😘
Gayle says
Why would Bob Snyder intentially report covid cases wrong or lower than they actually are? What is his intentions? Does he mean to damage the community or make it unsafe for school kids? Is he being paid off or some other ill intent? Please follow up.
Q says
Yes.. “19 new cases in one day” .. that was from – AT BEST – 5-7 … maybe 10 business days ago. That’s days old, but the best current, data. Just remember that: we are reading data that is 120-168 hours, or more, old. How many do you think became infected in anyone of those hours from the ones, the maskless vigilanties, who refused to quarantine? I’d bet, a few for sure. Now, please, lets let the naysayers with their “our immune systems are so strong” try to talk this down. Janet maybe? Please. Mic drop.
M says
Who cars how many people, including kids, get sick and possibly die? Let’s make sure we get them schools open.