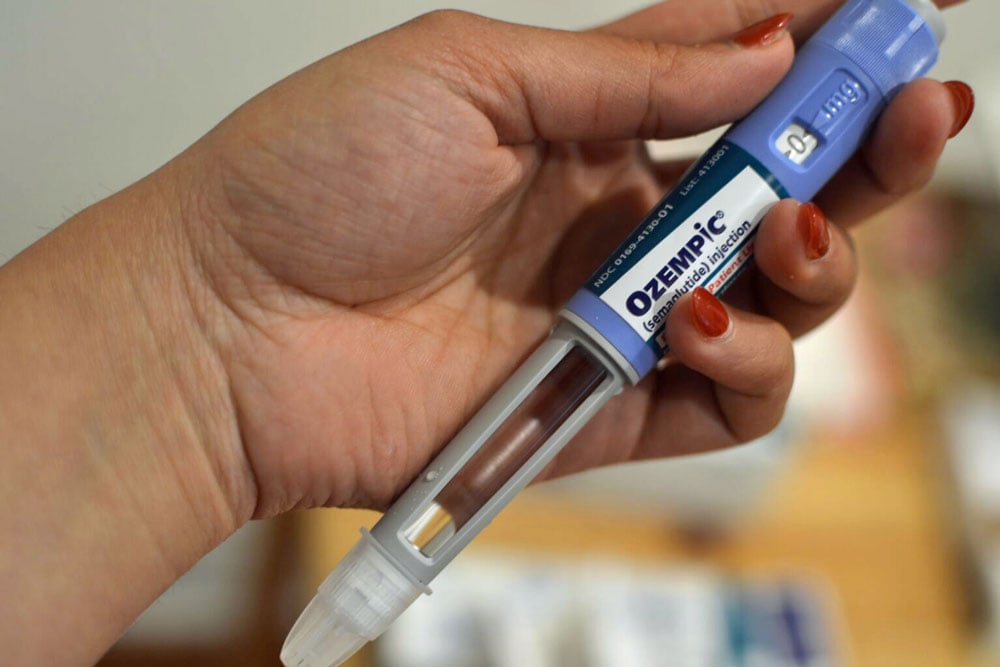
Massachusetts and Rhode Island are considering dropping GLP-1 drugs for obesity treatment from their Medicaid programs, continuing a trend of states that have stopped coverage of these expensive medications.
Thirteen state Medicaid programs are covering GLP-1 drugs for the treatment of obesity this year, down from 16 last year.
Medicaid programs in California, New Hampshire, Pennsylvania and South Carolina have eliminated coverage of the drugs for weight loss, because the expense strained state budgets.
In Massachusetts, the governor’s proposed fiscal 2028 budget would not fund the state’s Medicaid program, MassHealth, to cover GLP-1 medications for weight loss alone, though the state would continue covering the drugs for diabetes and other conditions. The legislature is still debating the state budget.
Rhode Island’s governor also has proposed removing GLP-1 coverage from the state’s Medicaid program for weight loss treatment.
North Carolina reinstated such coverage in mid-December after having dropped it in October.
Medicaid programs in Delaware, Kansas, Michigan, Minnesota, Mississippi, Missouri, Tennessee, Utah, Virginia and Wisconsin also cover the drugs for obesity treatment, according to KFF, a health policy research group.
![]() But some states, such as Michigan, have restricted eligibility for these medications to morbidly obesity patients rather than those who are overweight or obese. The move is expected to save the state an estimated $240 million.
But some states, such as Michigan, have restricted eligibility for these medications to morbidly obesity patients rather than those who are overweight or obese. The move is expected to save the state an estimated $240 million.
Meanwhile, lawmakers in Louisiana are debating whether to allow Medicaid to cover GLP-1s for obesity treatment if enrollees have another chronic condition, or comorbidity, such as prediabetes, hypertension or cardiovascular disease.
The medications generally have been too expensive for people without insurance. In February, one of the largest producers of these drugs, Novo Nordisk, announced it would reduce their list prices to $675 per month in 2027.
Gross spending on Medicaid prescriptions for GLP-1s — for diabetes as well as for weight loss — has increased from around $1 billion in 2019 to almost $9 billion in 2024 as demand for these drugs has risen, according to KFF.
At the same time almost 40% of adults and a quarter of children with Medicaid have obesity and may benefit from having access to the drugs, according to KFF.
–Shalina Chatlani, Stateline

























Pogo says
Still true (pun — and bun, intended)
https://www.google.com/search?q=penny+wise+pound+foolish
Related?
https://www.google.com/search?q=annual+expenditure+advertise+unhealthy+food+consumption
Gluttons being punished by the same people who promote and profit from gluttony; welcome to the circus we call home.
R.S. says
Obesity begins in childhood, when almost none can make sensible decisions about their diet. Penalizing someone for what they couldn’t control makes no sense. What we’d really need is a National Health Service, properly funded by taxes. Here’s a cost comparison: United States: $936; Japan $169; United Kingdom $93; Australia $87; France $83. How can they do it? Here’s the response from “Healthy Living magazine” Countries like the U.K., France, and Australia negotiate directly with drug manufacturers to keep prices in check. Their healthcare systems also centralize purchasing and have stricter pricing rules. In the U.K., Ozempic costs just $93 per month less than 10% of the U.S. list price. In France, the price dips to $83. Japan pays more than Europe, but still just $169 far below the U.S. average. [https://healthylivingmagazine.us/ozempic-prices-around-the-world/]. It’s a crying shame that we’ve got a person claiming to be a business dealer in the White House; yet we’re still being ripped off by the system, by way of which he profits.