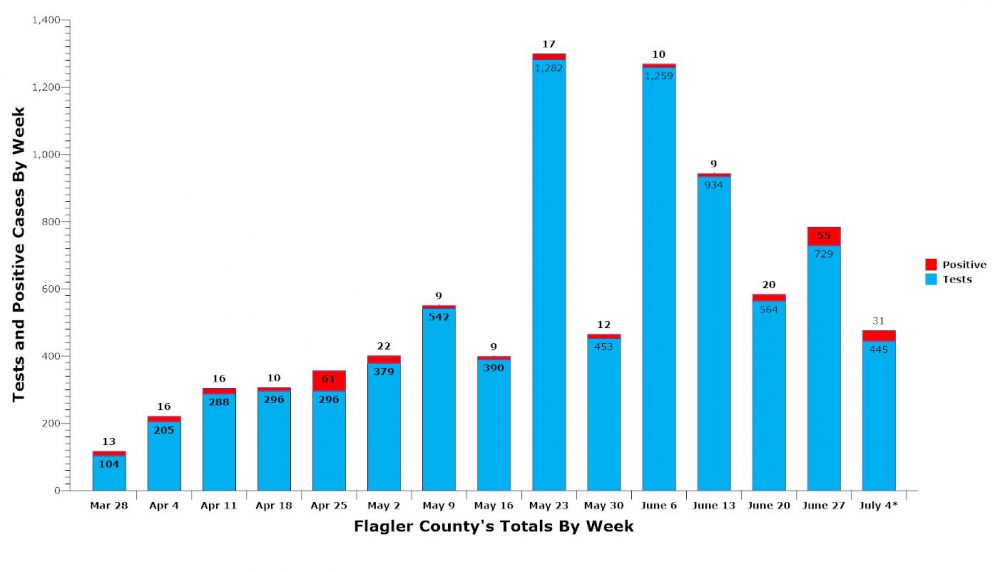
A resident at Princeton Village of Palm Coast, the assisted living facility off Belle Terre Parkway, is among the 31 Flagler County cases positive for Covid-19 the Florida Department of Health has reported in the last three days, six on Monday. The county recorded 55 new cases last week and a total of 115 new cases since Phase 2 reopening began on June 5 as the surge of coronavirus cases across Florida reached Flagler.
The new case at Princeton Village means two residents at assisted living or nursing home facilities have tested positive so far in Flagler. A resident at Tuscan Gardens was reported positive earlier this month. A staffer at Princeton Village had tested positive previously. A cumulative total of four staffers at four facilities have tested positive.
Three corrections deputies at the Flagler County jail have tested positive since the start of the pandemic. Only one is currently in isolation. No inmates, past or present, have tested positive, a sheriff’s spokesperson said Monday.
Flagler’s county-specific report from the state Health Department shows that 21 people in long-term care facilities and seven people in correctional facilities have tested positive. But the report is resident-specific. That means 21 people who live in Flagler and work in long-term care facilities, whether in Flagler or surrounding counties, have tested positive. Corrections personnel at Tomoka state prison or at the Volusia Branch Jail who have tested positive may be residents of Flagler.
The state reported just over 6,000 new cases on Monday, after reporting 5,400 on Sunday and 44,000 new cases last week. Cases in Florida have more than doubled since Gov. Ron DeSantis launched Phase 2 of the state’s reopening on June 5.
The state today reported 58 additional deaths related to Covid-19, for a total of 3,604, including 99 non-residents of the state. The number of deaths reported today is among the highest single-day totals in the last two months.
After a relative lull in May and early June, Florida’s cumulative total is now 152,400. More alarmingly, however, is the positivity rate–the rate at which those tested for Covid-19 are positive. The rate’s seven-day average had only very briefly exceeded 12 percent in the earliest days of the pandemic, when very few people were being tested, and again in late March and early April. It had fallen to well below 5 percent in mid-May. Since June 7, it has risen sharply to around 15 percent, pointing to widespread community transmission, including among young, asymptomatic individuals. That suggests a large number of people are walking around with the virus, not suspecting that they’re infected–but infecting others.
The positivity rate’s seven-day average in Flagler is 5.9 percent. But as in the rest of the state, weekly counts of influenza-like illnesses and Covid-like illnesses at AdventHealth Palm Coast’s emergency room have risen from just over 20 the week of June 14 to over 35 the week of June 21.
As of Monday, AdventHealth Palm Coast was caring for four Covid-19 individuals as in-patients at the hospital, Snyder said today.
In the state, the number of people reporting influenza-like illnesses in hospital emergency rooms rose from fewer than 2,000 the week of May 31 to around 5,000 the week of June 21. The number of people reporting Covid-like illnesses rose from just over 2,000 to over 8,000 in the same span.
Florida, along with Arizona, Texas and South Carolina, is among the leading new hot spots of the pandemic, with daily cases nationally rising beyond totals seen at the previous height of the pandemic in April. Hospitals in Houston are getting overwhelmed. That has not been the case in Florida, where bed capacity was at 22 percent today, according to the Agency for Health Care Administration. Intensive Care Unit bed capacity statewide is at 33 percent, the same number as at AdventHealth Palm Coast, where six of 18 ICU beds are available. The hospital also has capacity for immediate expansion of ICU beds should the need arise.
In Flagler, the median age of those testing positive has averaged 44 in the last two weeks (ranging between 26 and 71 during the period). Among 10 cases confirmed on Sunday, for example, ages five people were in their 20s, others were 41, 49, 51, 50 and 72. All were residents. Only two had recently traveled–one to New York, another to North Carolina, pointing to local transmission above all. The previous day, a 13-year-old girl and a 19-year-old woman were among those confirmed positive, along with people in their 40s, 50s, 60s and 70s.
Snyder said the department is continuing to stress four essential behaviors for residents: social distancing, facial covering, handwashing, and staying home if sick. The department is hiring 14 additional staff members to enhance community testing, primarily at long-term care facilities. Those facilities are under a state requirement that all staffers be tested every two weeks. Long-term care facilities have accounted for about a third of the state’s fatalities (between residents and staffers). The department is also continuing to focus on case investigations and contact tracing while furthering the messages it’s been dispensing for months. “All those messages haven’t changed. We just need to do more of it,” Snyder said.
The Institute for Health Metrics and Evaluation, whose Covid-19 model is closely watched by local officials, has revised its projections for deaths in the state, now expected to exceed 13,000 by October 1. The model revises projections based on current trends and behaviors. The absence of mandates such as mask-wearing or stay-home orders amplifies the likelihood of more infections and, consequently, more deaths. The model points to a wide disparity between expected deaths if masks are not mandated as opposed to expected deaths if they are mandated, with significantly lower numbers when masks are mandated. The projection for the United States is that deaths will exceed 175,000 by October 1 if current trends hold.

























LetThemEatCake says
All those people that tested negative need another test or five. Just because you test negative one day doesn’t mean you’re not positive. It means your body hasn’t produced enough of the virus for it to show on the test. I doubt people are going back and getting retested and retested so I’m sure there are many more cases out there statewide that we don’t know about. In addition, a certain percentage of tests produce false negatives/positives so really, testing is not absolute. I still don’t understand how the leading country in all things has failed so miserably at this response. South Korea bangs out tests. Stomps out clusters. The US? We can’t even wear masks to protect each other because too many people are selfish and don’t care about their neighbor, their co-worker, their friends, their relatives…it’s a sad world when someone can’t put a piece of cloth over their face for a short amount of time to protect someone else from them.
Mark says
What should we do? Beat people who refuse to wear a mask? Yes, they are very inconsiderate. Do we make “inconsiderate” a felony?
Gigi says
Homicide is a felony. If you don’t wear a mask, you could cause someone to get sick and die. You don’t have to be experiencing symptoms to spread the virus.
kcpc says
We must mandate face coverings. I’d like to know which of our council members oppose this and are endangering lives in our community .
Mike Cocchiola says
Well, we’ve run out of miracles, Clorox didn’t work nor did wishing it away. The coronavirus ignored the official lies and obfuscation (as did most of America), and heat and didn’t slow it down at all.
So where are we? The Republican south and west are infected and setting coronavirus records because they believed in all of the above. The world is shunning us because we’re toxic. And there’s no vaccine within sight. All we can do is wear masks and social distance ourselves from Republicans. They’ll be the ones yelling about their 1st amendment right to infect everyone around them and to get the virus themselves to show their fealty to Boss Trump.
David S. says
So True Thank You…
Gary R says
Coronavirus death toll is heavily concentrated in Democratic congressional districts https://www.pewresearch.org/fact-tank/2020/05/26/coronavirus-death-toll-is-heavily-concentrated-in-democratic-congressional-districts/
Yellowstone says
Is there any online site that will indicate the COVID ‘hot spots’ in Flagler County? Palm Coast?
Percy's mother says
Florida Department of Health.
Up in the left-hand corner, there’s (in bold) info about Covid.
Click on that.
Scroll down all the way until you get to the “dashboard” box. Click on “dashboard”
Once in the “dashboard”, at the bottom you can click “by County”. Put in Flagler (that is in the box at the top right hand side of the table, and then once the Flagler County info has registered, again at the bottom “by zip code”.
You will be able to see the number of cases by zip code.
You can then decide where the “hot spots” are in Flagler County and Palm Coast.
Hope this answers your question.
Kim says
Yellowstone,
This website, updated daily, gives the data by county and also by zip code:
https://experience.arcgis.com/experience/96dd742462124fa0b38ddedb9b25e429
And, yes, before people complain, I know that the Florida website has its faults, but it’s at least daily info.
Dealk says
Aren’t the positive antibody test results mixed into the Positive Covid test results? A while back it was reported that they were combined. I wonder how many of Flagler County results were antibody? Well, for all of Florida for that matter.
Bob says
Again I ask. How many of those infected are now virus free???
Gigi says
You can be positive for up to six weeks. Some longer. Testing here in Flagler County can’t even keep up.
Only Me says
Governor DeSantis follows in Trump’s shoes since he worships him over the health of the people in the State of Florida. DeSantis refuses to make it mandatory for people to wear masks though the medical professionals state it is the safety for everyone to keep our economy opened.
DeSantis has failed to people and guests of Florida as well as Donald Trump has failed the people of the USA.
Both their ratings are hitting an all-time low and they have no business being in politics if they only care about themselves.
Both of them continue dumping the responsibility on the towns and states, that is what lack of leadership.
They both will want your vote at the re-election time but they way they are going I doubt few will be voting for either of them.
Local says
How can they come up with these numbers?i go by the supossed testing site almost every day and noone is there. They have a number to call and you cant even get an appointment. It will all disappear after the elections. It always does. Stop watching mainstream media.