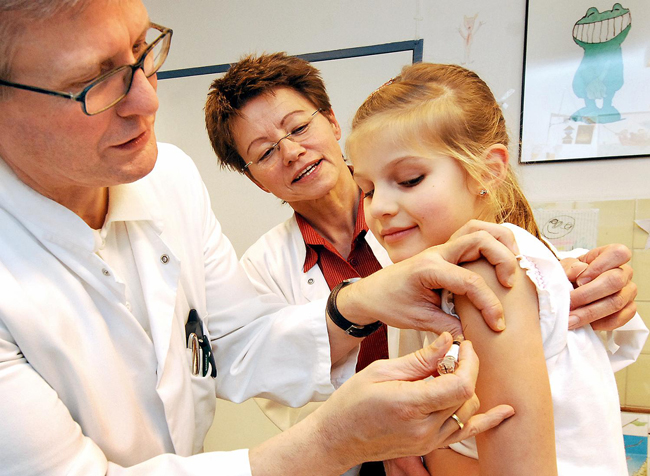
The human papillomavirus–HPV— is the most common sexually transmitted infection in the United States and a principal cause of cervical cancer. But its prevalence dropped by half among teen girls between 2006 and 2010, from 7.2 percent among girls ages 14 to 19 to to 3.6 percent.
Health officials attribute the drop directly to the HPV vaccine, even though in the United States parents are far more resistant to vaccinating their daughters than they are in other countries. That resistance is growing. While vaccination rates in some European and African countries is around 80 percent (including in countries as varied as Britain, Denmark and Rwanda), a study published in March found that 44 percent of parents in 2010 said they would not immunize their child against HPV.
Parents cite fears that the vaccine could have dangerous side effects. The fears are baseless, but have led to a significant drop in HPV vaccination that worries health officials. Friday, the Centers for Disease Control produced hard numbers about that drop.
HPV vaccination rates in girls aged 13-17 years actually failed to increase between 2011 and 2012, according to the latest CDC data. Three-dose coverage (the vaccine is administered in three doses over period of many months) actually declined slightly from 2011 to 2012. (The vaccine is for both boys and girls.)
Among girls un-vaccinated for HPV, 84 percent had a healthcare visit where they received another vaccine (such as one aimed at meningitis or pertussis) but not HPV vaccine, suggesting that the prejudice against HPV is not necessarily associated with a fringe but persistent prejudice against vaccines. Rather, it is the result of unsubstantiated assumptions among parents that vaccinating a girl for HPV would encourage promiscuity or accelerate the beginning of sexual activity. Such assumptions are more sexist and harmful, health-wise, than accurate: among girls who receive the HPV vaccine, there is no correlation between injections and the incidence of sexual activity.
If the HPV vaccine had been administered to those showing up for other vaccines between 2010 and 2011, the CDC found, vaccination coverage for one or more doses dose could be nearly 93 percent rather than 54 percent.
Approximately 79 million Americans are currently infected with HPV. About 14 million people become newly infected each year. HPV is so common that nearly all sexually-active men and women will get at least one type of HPV at some point in their lives.
“Progress increasing HPV vaccination has stalled, risking the health of the next generation,” said CDC Director Tom Frieden M.D., M.P.H. “Doctors need to step up their efforts by talking to parents about the importance of HPV vaccine just as they do other vaccines and ensure its given at every opportunity.”
According to CDC, for each year that HPV vaccination coverage remains near the current level of 33 percent instead of achieving the goal of 80 percent coverage, an additional 4,400 women will be diagnosed with cervical cancer and 1,400 cervical cancer-attributable deaths will occur in the future.
But much of that blame lies not just with parents, but with physicians and other health care providers who neglect to be forthright about the HPV vaccine.
The 2012 National Immunization Survey Teen data show that not receiving a healthcare provider’s recommendation for HPV vaccine was one of the five main reasons parents reported for not vaccinating daughters. The CDC actively urges healthcare providers, including local health departments, to give a strong recommendation for HPV vaccination for boys and girls aged 11 or 12 years.
The other responses parents provided indicate gaps in understanding about the vaccine, including why vaccination is recommended at ages 11 or 12.
“Parents need reassurance that HPV vaccine is recommended at 11 or 12 because it should be given well in advance of any sexual activity,” said Dr. Frieden. “We don’t wait for exposure to occur before we vaccinate with any other routinely recommended vaccine.”
Parents also reported safety concerns as a reason for not vaccinating. But in the seven years of post-licensure vaccine safety monitoring and evaluation conducted independently by federal agencies and vaccine manufacturers, no serious safety concerns have been identified. So-called “adverse events” to the vaccine have steadily decreased from 2008 to 2012 and the numbers of serious adverse events reported has also declined since 2009.
Parents and caregivers are encouraged to ask about vaccination every time they take children for a healthcare visit, especially for preteen boys or girls. For many, it’s easier than ever to get the HPV vaccine. Because of the Affordable Care Act, most private health insurance plans must cover the HPV vaccine at no out-of-pocket cost, meaning no co-pay or deductible.
CDC officials urge healthcare providers to increase the consistency and strength of how they recommend HPV vaccine, especially when patients are 11 or 12 years old. Reviewing vaccination status at every healthcare encounter and taking advantage of every visit, including acute care visits, can increase HPV vaccine coverage in the United States.

























foghorn leghorn says
People that refuse to get their kids vaccinated against HPV deserve to get cervical cancer.
Dolorosa says
If they aren’t harmful then why is this happening to young people? Recently in Florida, two teens from the same family came down with serious vaccine injuries from Gardasil vaccinations.
Learn more: http://www.naturalnews.com/030782_HPV_vaccinations_side_effects.html#ixzz2aHo6zkST
Pat says
Big Pharma and those who get paid to peddle their products will not be using my kids as human guinea pigs…
We need to talk about HPV vaccination – seriously (16 September 2011 by Charlotte Haug)
(http://www.newscientist.com/article/dn20928-we-need-to-talk-about-hpv-vaccination–seriously.html?full=true&print=true#.UfRru234JSk)
Should we vaccinate girls against HPV? Michele Bachmann’s blundering aside, there is no clear answer.
Why? First, there are more than 100 different types of HPV, at least 15 of which cause cancer. But the vaccine protects only against the two most important cancer-causing strains, HPV-16 and HPV-18, though it may also offer partial protection against some closely related strains (The Lancet, vol 374, p 301). But the remaining strains still cause cancer.
The HPV vaccine is designed to prevent cervical cancer, which currently kills around 250,000 women a year worldwide. It works by inducing immunity to HPV, the leading cause of the disease and the world’s most common sexually transmitted infection: around 79 per cent of people catch it at some point in their lives. Almost all infections are quickly cleared by the immune system, but in a few women infection persists and can progress to precancerous lesions and eventually cervical cancer.
There is another serious question that may be answered sooner: what effect will the vaccine have on the other cancer-causing strains of HPV? Nature never leaves a void, so if HPV-16 and HPV-18 are suppressed by an effective vaccine, other strains of the virus will take their place. The question is, will these strains cause cervical cancer?
Results from clinical trials are not encouraging. Vaccinated women show an increased number of precancerous lesions caused by strains of HPV other than HPV-16 and HPV-18. The results are not statistically significant, but if the trend is real – and further clinical trials should tell us in a few years – there is reason for serious concern.[…]
Ron says
You can thank Michele Bachmann for some of the HPV vaccine misinformation that’s floating around out there.
Barbara says
IMO….any parent who agrees to the HPV vaccination for their child should be charged with child abuse.
Sherry Epley says
Michelle Bachman’s usual Republican scare tactics aside. . . this from the US Center for Disease Control:
HPV Vaccine Safety
HPV vaccines were studied in thousands of people in many countries around the world, including the United States. These studies showed NO SERIOUS SAFETY CONCERNS and found that both HPV vaccines were safe. Common, mild adverse events reported during these studies include pain where the shot was given, fever, dizziness, and nausea. More than 46 million doses of HPV vaccine have been distributed in the United States as of June 2012. Most doses distributed have been Gardasil.
Syncope can occur after any medical procedure, including vaccination. Recent data suggest that syncope after any vaccination is more common in adolescents. Adolescents and adults should be seated or lying down during vaccination. Providers should consider observing patients in seated or lying positions for 15 minutes after vaccination.
For each of the vaccines, a detailed post-licensure safety monitoring plan, coordinated by the FDA and CDC, is in place. For more information about the Vaccine Adverse Event Reporting System (VAERS) visit http://www.vaers.hhs.govExternal Web Site Icon
HPV Vaccine Efficacy Studies and Antibody Response
The main efficacy study of the bivalent vaccine was conducted in young women aged 15 through 25 years. Among women who had not been previously exposed to a targeted HPV type, the clinical trials demonstrated 93% vaccine efficacy in preventing cervical precancers due to HPV 16 or 18. In all studies of the bivalent HPV vaccine, more than 99% of females developed an HPV 16 and 18 antibody response 1 month after completing the 3-dose series.
The main efficacy studies of the quadrivalent vaccine were conducted in young women and men (16 through 26 years of age). Among persons not previously exposed to a targeted HPV type, the trials demonstrated nearly 100% vaccine efficacy in preventing cervical precancers, vulvar and vaginal precancers, and genital warts in women caused by the vaccine types, as well as 90% vaccine efficacy in preventing genital warts and 75% vaccine efficacy in preventing anal precancers in men.
In women already infected with a targeted HPV type, the vaccines do not prevent disease from that HPV type but protect against other vaccine types. Immunogenicity studies of both vaccines have been conducted in girls, ages 9 to 15 years of age. Over 99% of vaccinated girls in these studies developed antibodies after vaccination.
HPV vaccines offer a promising new approach to the prevention of HPV and associated conditions. However, they do not replace other prevention strategies, such as regular cervical cancer screening using the Pap test, since the vaccines will not prevent all HPV types.