In the wake of a death in Flagler and two cases in Volusia County, the Flagler and Volusia county health departments have issued an advisory against eating raw shellfish or seafood or wading in the Intracoastal’s brackish waters if you have lesions, to avoid catching a cholera-like, flesh-eating bacteria.
Henry Konietzky, 59, is the latest victim to die from exposure to the bacteria. The Flagler County resident was setting crabbing traps in the Intracoastal in Ormond Beach. He was infected Saturday. He died Monday. “unfortunately it pretty much overwhelms the immune system,” Patrick Johnson, director of Flagler County’s health department, said.
He is the ninth person to die from the bacterium in Florida this year. Twenty-six cases have been reported. An epidemiologist found that in August a man crabbing in the same vicinity where Konietzky came down with it had also been exposed to the bacterium. That’s what led the health department to issue the advisory.
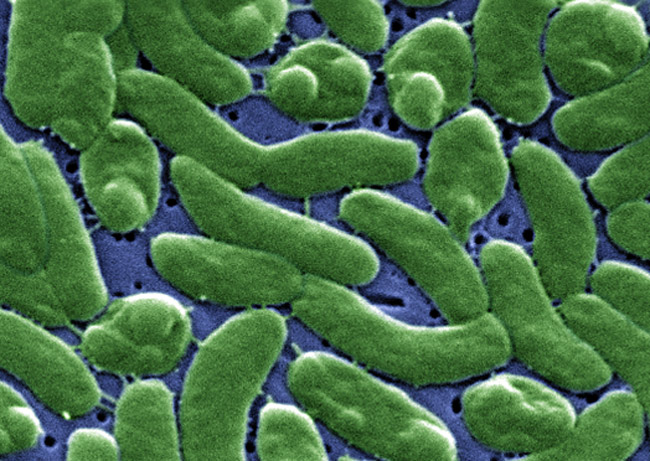
The bacteria is called Vibrio vulnificus, and is in the same family as those that cause cholera. It normally lives in brackish seawater and is part of a group of vibrios that are called “halophilic” because they require salt.
“We’re not talking about the ocean here, we’re really talking about Intracoastal type of area,” Johnson said. “But it normally is in this type of area, and it’s naturally found there, so there’s no way of eliminating it.”
The most common means of infection is by eating raw oysters contaminated with the bacetria. Exposure through an open wound is another way. The symptoms of exposure are vomiting, diarrhea and abdominal pain if infection results from eating contaminated fish. If exposure occurs through lesions, a fever rapidly progresses to septic shock. It is especially damaging to people who suffer from liver disease. Bloodstream infections are fatal about 50 percent of the time, the Centers for Disease Control report.
“Number one, cook seafood. Don’t eat raw oysters or raw shellfish, clams and mussels,” Johnson said. “They should be cooked thoroughly. Then when you’re doing the crabbing type of business if you have any type of lesion on your leg or your hands even if you’re getting your hands dirty with brackish water, I would avoid it until you are healed or do it from the shoreline.”
Wear protective clothing such as gloves when handling raw shellfish. When cooking shellfish, either boil until the shells open and continue boiling for five more minutes, or steam until the shells open and then continue cooking for nine more minutes. Do not eat shellfish that do not open during cooking. Boil shucked oysters at least three minutes, or fry them in oil at least 10 minutes at 375°F.
Avoid cross-contamination of cooked seafood and other foods with raw seafood and juices from raw seafood. Eat shellfish promptly after cooking and refrigerate leftovers.
The CDC reports that Vibrio vulnificus is a rare cause of disease, but it is also underreported. Between 1988 and 2006, CDC received reports of more than 900 Vibrio vulnificus infections from the Gulf Coast states, where most cases occur. Before 2007, there was no national surveillance system for Vibrio, but CDC collaborated with the states of Alabama, Florida, Louisiana, Texas, and Mississippi to monitor the number of cases of Vibrio infection in the Gulf Coast region. In 2007, infections caused by V. vulnificus and other Vibrio species became nationally notifiable.
Although oysters can be harvested legally only from waters free from fecal contamination, even legally harvested oysters can be contaminated with the bacteria because it is naturally present in marine environments. The bacteria does not alter the appearance, taste, or odor of oysters. Timely, voluntary reporting of infections to CDC and to regional offices of the Food and Drug Administration help collaborative efforts to improve investigation of these infections. Regional FDA specialists with expert knowledge about shellfish assist state officials with tracebacks of shellfish and, when notified rapidly about cases, are able to sample harvest waters to discover possible sources of infection and to close oyster beds when problems are identified. Ongoing research may help the CDC to predict environmental or other factors that increase the chance that oysters carry pathogens.
For more information, please visit the Centers for Disease Control and Prevention website.




























Aquaman says
Increased water temperatures are causing this. No hurricanes to clean out the brackish waters. So is the planet warming or is it cooling ? Or is all the heat being sucked into the oceans as a heatsink. Fishing is the worsted its been in 50 years of ocean fishing. Algae’s growing EVERYWHERE and becoming more toxic to both marine life and humans. What gives ?
A.S.F. says
This is extremely scary!
rhweir says
There is no outlet to the ocean in Flagler County so most boat owners are confined to the ICW. This is interesting information and should have been released much earlier if the bacteria has been a problem all summer. I had a run in with a catfish last summer while unhooking it and was finned, had a reaction and ended up in the ER. While I didn’t develop vibro, the staff at the ER kept telling me to watch it and report any illness. Now I know why. I did suffer from vibro while in N California a few years ago from mussels and believe me, you do not want that, it’s very difficult to recover from and I almost died. I’d like to see a follow up piece and what seafood is affected, what about water skiing, crabs as well as shellfish and what about fin fish. Flounder and snapper are biting in the ICW and being taken, eaten and sold in local markets.
Ray Thorne says
I’m not much of a seafood eater but I do love the water. After the first article came out i had gone up to Matanzas Inlet… no one was there. Scary stuff indeed.
The Doctor says
It’s here every year, nothing really new. It is just very unfortunate that someone died from it locally. But it’s nothing new at all. It has been a factor in the south for years.
randy irwin says
why then did the news journals reporting target high bridge as the area where this happened……….It certainly will not help the business’ in the area.in my opinion it was shabby reporting and could have been more specific and informative———————–or am I to critical ??? v-vet
rhweir says
http://www.ecolab.com/our-story/our-company/our-vision/safe-food/microbial-risks/vibrio
Vibrio link.
NortonSmitty says
Well, there were two crabbers wno got sick in that particular area. And the only business I know of within two miles or so is the bait shop. So maybe too critical. We won’t hold it against you this time.
Katy says
We are new to Florida/Palm Coast. Is this something that happens seasonally? Will it become less of a threat at any point?