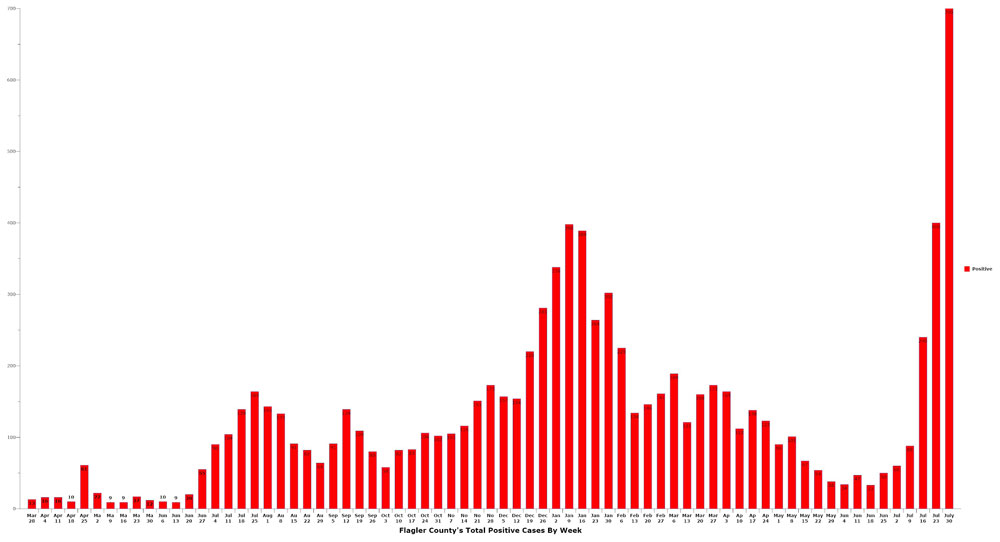
While the Flagler Health Department and AdventHealth Palm Coast are overrun with Covid cases and in-patients, local governments have gone silent, indifferent to the worst wave of the pandemic yet, making a mockery of their claim of a “partnership” with the Health Department or the hospital and amplifying community apathy that multiplies infections.
This is the crisis hospitals and public health agencies have feared since the beginning of the pandemic. It did not overwhelm hospitals and health departments in the first three waves. It is overwhelming them now. And unlike previous waves when health workers were lionized and local governments championed their health departments, no one is doing so this time around. In Flagler especially, the Health Department and AdventHealth Palm Coast are fighting this one on their own.
The unvaccinated continue to refuse to be vaccinated: despite record-breaking numbers day after day, the vaccination numbers are barely budging, reflecting the gravest indication of indifference from the segment of the community that could be battling the fourth wave, and future waves, most effectively.
There is no big, ominous tent outside the emergency entrance at AdventHealth Palm Coast, as there was in the earliest days of the Covid pandemic, when hospitals feared being overrun with patients. But there are scores of chairs lined up outside the ER. Wednesday night, the ER inside and out was full, and 60 beds in a hospital licensed for 130 were filled with Covid-19 patients, almost twice the record set last January, and double the number from barely a week ago.
There are now 1,000 covid patients in AdventHealth’s 16 hospitals in the Central Florida region, a record. And on Wednesday alone, 139 covid infections were confirmed in Flagler County–a number that previously had been alarming enough when it reflected a weekly total. This week’s infections, when confirmed on Friday, are on pace to be in the 700 range, shattering last week’s record 400 infections.
“I went to the ER in Palm Coast, but when I saw the scene was like a hospital in Gaza, I turned around and came home,” Rick de Yampert, FlaglerLive’s culture writer, said of his experience Wednesday night, when he went to the ER at 9:45 p.m. He’d been battling a urinary tract infection. It had gotten worse. He needed to see a doctor.
He saw this instead: “There was a giant, a huge RV-looking vehicle, and right behind it was a Ford Explorer, one of those type trucks, and I could see in the street lights, each of them had a ‘Covid Response’ banner on them. I got out, I went to the entrance, a woman came up to me and said, ‘Can I help you?’ and I said it doesn’t look like you can, because it looks like you’re being overrun.” By then he’d seen inside the waiting room. “It was people everywhere I looked, it was socially distanced but I didn’t see an empty seat, and outside they had chairs, and eight or 10 people were sitting there. One of the security guards was trying to calm down an elderly man who didn’t want to sit in the chairs.”
Between the people inside and outside, de Yampert estimated 30 were waiting. “It was kind of unnerving, like, fuck, what if I had a more serious thing–what if people there had serious [issues],” he said. (He saw his doctor in Ormond Beach this morning.)
On Wednesday, there were 107 Covid patients in Advent’s Daytona Beach hospital, 162 in Orlando, 31 in New Smyrna Beach, and 112 at Altamont, among other Advent locations. A new phenomenon: multiple unvaccinated, pregnant women in intensive care, some on ventilators, according to AdventHealth spokesman Jeff Granger, with disturbing consequences for gestating babies’ development. Flagler County’s public health department, itself overrun, is scrambling to add case investigators and contact tracers while revamping its testing and vaccination operations to make them more efficient during the crisis.
Yet for all the sense of crisis within hospitals and public health departments, the community bat large has been mostly indifferent: vaccinations in Flagler County continue to lag to the point that the Health Department is closing its three church-based vaccination sites, which were drawing only three or four people willing to be vaccinated each of the days they were open. Local governments are proceeding as if this were just another summer. Palm Coast and county governments in earlier points of the pandemic were focused on safety messages and measures. The last few days, they’ve been issuing smiley-faced news releases about sewer plants, a “litter pick-up” event on Saturday, a feature on the county’s emergency helicopter or boasting about commissioners’ awards. The school district is preparing for a full opening of schools on Aug. 10 without mask requirements or learning options other than in-person (the usual virtual school option aside). Flagler’s Tiger Bay Club just announced its August wine tasting event, in-person of course (but outside, under a tent).
It’s two parallel worlds. A few businesses are restoring masking mandate (Disney did so in Orlando on Wednesday, for all visitors, whether vaccinated or not, at all times), but Gov. Ron DeSantis continues to fight all local covid-safety measures, including masking or vaccine checks.
In contrast with earlier covid waves, not a single local government has sent out public advisories urging safety or cautionary measures. Not a single local government has issued vaccine advisories. Not a single elected official, in the county, on municipal boards or on the school board, has used his or her seat to urge vaccination.
On the face of it, the governments continue to call themselves partners with the local Health Department. In fact, the Health Department is now battling the public health emergency alone, while the hospital is contending with it as if ghettoized from the rest of an indifferent community.
The increase in Covid cases in Flagler are affecting “all age groups, with the largest increases in the younger age groups,” Bob Snyder, the Flagler County Health Department chief, said. “So this is now requiring a shift in our strategy. We’re just going to have to reprioritize ourselves to focus on the most vulnerable in our community. That would include of course our seniors immunocompromised, and especially our kids now that school is going to be returning on August 10. Individuals under the age of 12 are not vaccinated, so we consider our children’s school aged children to be among the most vulnerable. ”
The testing and vaccination will take place at Health Department headquarters at at 301 Dr. Carter Boulevard in Bunnell and at the department’s annex, especially since the school district has agreed to cooperate with the department in the rapid-covid-testing system for teachers and students. That rapid testing will reduce the number of staffers and students who need to quarantine, as long as they test negative after exposure to other confirmed cases.
But the department is trying to cope with a surge it has not previously experienced. “It’s overwhelming,” Snyder said. “We’ve added staff. We have staff that were maybe not working a full 40 plus hour week, were OPS staff, they now are again.” (OPS is a human resources acronym that stands for Other Personnel Services.) So thank God we have a little stable of individuals at the ready to commit to longer hours, plus we have put in through a special manpower request for five additional case investigators and contact tracers.”
At this morning’s briefing on Covid, AdventHealth’s physicians tried to put in words the unprecedented in an 18-month pandemic that’s mutated the unpredictable.
“We’ve seen waves occurring, of course, since the beginning of the pandemic, with the most recent large wave being in January,” said Dr. Vincent Hsu, executive director of infection prevention and epidemiologist at AdventHealth. “Our current wave that we are seeing is actually exceeding and past the numbers that we had seen in January, and what’s extraordinary is the speed at which we are currently seeing new cases. And unfortunately right now, the slope is pretty steep, and we haven’t seen the end of it.” He added: “It is going to get better, clearly it’s going to get better. I don’t have a crystal ball as to when. I think we have to recognize that the delta variant behaves in ways that were unlike the other variants and so this is a significant issue that we’re going to have to deal with.”
The hospital system has again narrowed the visitor policy to one visitor per patient, whether Covid or not, except for children, who may have two visitors at a time. Earlier this week, the Centers for Disease Control changed its mask recommendation, again pushing masking indoors even for those who have been vaccinated. This applies in areas of high transmission. “That really includes the entire state of Florida, Hsu said. “That’s what we’ve been doing at AdventHealth in our facilities, and it is something that we should follow–we should follow the advice of the CDC until we get more data on this. But I also want to emphasize: mask wearing is something that we would recommend even if you are vaccinated, but for those that are unvaccinated, really consider getting vaccinated. This is really one of the reasons why we have had spread is we’ve had so have a large number of unvaccinated. That is the single best way that you can do to protect yourself and prevent spread.”
Masks, he said, can only help. Disinformation aside, they do not hurt.
With “Gaza”-like scenes at emergency rooms such as the one described above, AdventHealth officials are urging patients who are not requiring oxygen or are significantly short of breath, “the way to be tested is in the outpatient world,” says Dr. Michael Cacciatore, chief medical officer of the AdventHealth Medical Group. “Our primary cares in our group have testing, rapid testing done available in their offices. We can get tested at CentraCare, there are government places that you can be tested as well. And we even have some drive thru for our AdventHealth medical group patients that we can know where you’ve been seen by telehealth, that don’t want to go into an office but want to stop and get tested. So there are a lot of options out there and [emergency rooms] should be the last choice.”
Significant illness is described as inability to catch one’s breath or taking a few steps without feeling exceptionally short of breath. With those signs, a visit to the ER is recommended. Some patients can now be given monoclonal antibodies, which block the development of the illness as long as the injection–essentially, a 30-minute IV drop with monoclonal antibodies–is provided within the first 10 days of infection. Those patients show remarkable success fighting the infection and keeping it from becoming grave.
There is no question, however, that “breakthrough” infections–infections of people who have been vaccinated–are happening. But wearing a mask and distancing is another way to prevent breakthrough infections, which nevertheless are very unlikely to degrade into hospitalizations and intensive care requirements.
Florida meanwhile has become the nation’s epicenter of the epidemic–again. There are no equivalent measures of epicenters of misinformation. But local officials are battling that, too–and the complete vacuum of solid, public health information from local governments, which disinformation finds easier to fill.
“It is just very, very frustrating. There’s so much misinformation out there,” Snyder said. “And all we can do as public health officials and as scientists and researchers and the medical community, physicians, all of us, we just need to continue to just share the truth, share the data, and just provide our common sense, public health recommendations that have been identified as evidence-based and just validated by the medical community in general. We just need to keep communicating and identifying the reasons why folks need to get vaccinated and hope that minds get turned. And again, be available to have open discourse and answer questions. You know, this thing has been politicized. And so that definitely is an obstacle. but I don’t think it’s one that us public health officials can overcome.”



























Resident says
Wear a mask people and get the vaccine, please – our lives depend on this!
David S. says
Totally agree tell the republicans this. Just take a minute and listen to these clowns in congress you will be shocked.
Concerned Citizen says
Stop blaming Republicans.
I know many democrats who aren’t vaccinated and choose to not mask. This is more a personal responsibility thing. We are past pointing fingers and yelling at each other. Time for ALL parties to step up and do what’s right.
Just as we were getting to be OK I now have to watch my wife who is a Physicians Assistant go back to working 16 hour shifts and coming home a wreck. So it’s personal to me.
Ray W. says
I agree with Concerned Citizen that we ought to be long past pointing fingers and yelling at each other, but the problem is that both Republicans and Democrats in significant numbers are still neither getting vaccinated nor wearing masks. Yes, the balance is skewed towards Republicans being the vast majority of those refusing to get vaccinated or to wear masks. And don’t count out those who have rejected both political parties.
Perhaps, the better approach is to continue blaming Republicans who refuse to get vaccinated or wear masks – and their leaders – and add the much smaller number of refusing Democrats to the mix. As an aside, I spoke with a retired acquaintance today about a number of things, including his rescue Chihuahua (I have three). He shared his decision to finally get the first shot. He spoke of having to wait three weeks to get the second shot. He seemed resigned to the decision, certainly not as eager as those I spoke with in the early stages of the vaccine distribution scheme; they were all proud to have taken the effort. At least, anecdotally, the message is getting through.
Thinking that people who previously declined to be personally responsible will suddenly do an about face, or “step up” as Concerned Citizen puts it, is wishful, at best. Personal responsibility is a wonderful mantra. I spent over thirty years prosecuting and defending people charged with crimes.
I decided a long time ago that relying on the mantra of personal responsibility for other people is a waste of time and effort. Some people decide right and wrong by asking themselves whether they want to do something. If they want to do it, it is automatically right. If they don’t want to do it, it is automatically wrong. Since what they want to do changes every day, right and wrong changes every day, too. Just read some of the comments on FlaglerLive! Food prices have tripled, one commenter claimed. Apparently, he just wanted to claim something and saying prices tripled sounded good in his mind, so he typed it into a comment. People shout vulgarities and approach motorists on street corners near parked trucks displaying vulgar signs, all the while believing in the Big Lie! How many Republicans now say there may soon come a time when they have to take up weapons against our government? Even after the January 6th insurrection! And Republicans have long claimed they belong to the party of personal responsibility. How many voters in the recent mayoral race voted for Lowe? 25%? And already people are making noise about election fraud? All without a whit of personal responsibility. In the vernacular of Thomas Reid, are any of these people even educable?
As I repeatedly told my four children: There are only two questions. Do I have to do it? Do I want to do it? First, always ask whether you have to do it. If yes is the answer, never ask the second question. If no is the answer, then you can question whether you want to do it. Ordinary people do what they want to do. Extraordinary people do what they have to do.
Do people who present to the ER with Covid symptoms still deny the existence of the virus? How could anyone persuade these people to step up and get vaccinated and wear a mask?
Kat says
The next to the last paragraph is something framable. Wise guidance on your part, thank you for sharing.
S.David says
Tell your Black democrats they need to get vaccinated.
Makeitso1701 says
For every “black democrat” there’s probably 1000 trumpsters that refuse to get vaccinated. Their source of misinformation is the propaganda fake fox news.
I hate to put this way but, there will be less trumpsters that will be voting in the coming elections. Think about that, maybe that will be a motivation to get vaccinated.
Karen Curry says
Shhhhh Makeitso1701! Let the covidiots/trumpsters choose their poison. The only downside to it is that they will take some innocent bystanders with them, not that they’ve ever given a thought to the collateral damage they cause while claiming they are exercising their ‘freedoms’.
CC says
As soon as you tell your white redneck friends to vaccinated!
Marge Calcara says
I am a Republican and all my family and friends that are also Republican are vaccinated, wear mask in crowds and act responsibly. I don’t know where you get your info but you are wrong. Just because most do not think it should be mandatory we do what is right, the government does not have to tell us what to do.
Everybody needs to use common sense, I still use Walmart online food ordering and pick it up, no contact at all. We have choices.
FB says
If you notice in this whole story they do not tell you the percentage of people in the hospital that are vaccinated. In the past they have done this, but now they are leaving this very important data point out. I would assume that is because it is not just one percent of the folks in the hospital for Covid reasons like they have claimed in the past. This would give ammunition to the folks not wanting to get vaccinated. When you leave this out it tells me vaccination is not gonna do any good!
FlaglerLive says
FB is incorrect. The vaccinated percentage hospitalized is in the 1-5 percent range. From AdventHealth on July 22: “Approximately 95% of 12,700 COVID-19 patients treated this year across AdventHealth’s 41 hospitals in seven states were unvaccinated or partially vaccinated.”
BF says
Flaglerlive,
FB is incorrect? The data that you give has two problems. The first is July 22 was seven days ago and according to you all this huge number of folks in the hospital has happened over the past week. Secondly, the data that you’re describing about the year to date hospitalizations at 95% for the unvaccinated makes no point at all. In January very few people were vaccinated and also the Delta variant has only become the dominant version in Flagler in the last few weeks. Tell me what the percentage is today in the hospital of vaccinated versus unvaccinated. My guess is you will not answer the question as you did not in the response above. There is a reason why you’re not answering as it will not back up claim and FB will be correct.
FlaglerLive says
Let’s take the bait and address this despite a heckling tone that betrays more trolling than thoughtfulness. The stats up to July 22, or just over a week ago, are the latest available, and pretty conclusive about six months of hospitalizations (more than 12,000). As soon as new stats are available, they’ll be reported. But what’s your game here? To suggest that suddenly the vaccine is not as effective as advertised? That all the hospitalized of the last two weeks are vaccinated? Let’s say the more recent delta-struck proportion is not 95 percent. Let’s say it’s 90 percent. For argument’s sake, let’s say it’s 80, or even 70 percent. Are you suggesting that a lower proportion of effectiveness, while still very high, somehow undermines the message about the vaccine’s importance? What are you, cheering for going unvaccinated because 70 percent isn’t good enough for you? You’re willing to have people gamble with their lives even if they can win 70 percent of the time? Again, that’s assuming only for argument’s sake that the effectiveness ratio falls that blow, which it very doubtfully will. The message would still be the same, just as it is with masks, which provide significant protection but nowhere near full-proof protection, though masks in combination with vaccines are quite the armored option. But you’re not coming at this from an intellectually honest perspective (just as you pretend that “FB” is a different person than you, when it isn’t). We’re taking the time to address it, wasteful as the task may be, to better inform readers about those other delta variants of misinformation that you carry so well. You threaten in another comment that you’ll take your case to Facebook: go to it. That’s where disinformation thrives. But spare us your trolling. It’s not accepted here. Thanks.
Update: AdventHealth physicians at their 1 p.m. media briefing today revealed that 6 percent of those hospitalized currently are vaccinated. “99 percent of our deaths are also now in our unvaccinated population,” says Dr. Neil J. Finkler, Advent’s chief clinical officer.
MK says
A trip to the ER for the very ill is a dangerous endeavor this week because they have had to sit in the same waiting room as COVID patients (who refuse to put their masks over their noses) for up to 4 hours. If you suspect you have COVID because one of your 7 family members has it please stay home or go to an Urgent care center to get tested. The only reason to come to the ER is if you are short of breath when taking a few steps, have a temperature greater than 102 despite taking Tylenol and Advil, have a rapid heart rate, or a low blood pressure.
John Stove says
You can thank Fox News, Tucker Carlson, Republicans, Trump and his cult for continuing to push the misinformation that vaccinations and masks are an “attack on my personal freedom”….run the numbers, most infected people are the unvaccinated.
Your “personal freedom” is going to cost you a lot of money to be hospitalized and if you are lucky enough to survive the disease with no side effects perhaps you will come to your senses.
If not then there is no fixing stupid.
David S. says
You know when you have a Gov and those clowns in Washington who could care less about us . All they are worried about is there name, making money and getting reelected nothing will never get done. These non vaccine people are giving a big FU to everyone else its so sad. Nothing even from the City of Palm Coast…..
The dude says
Was just talking to my wife.
If something doesn’t change in the next week or two, my ten year old will not be walking in the doors of Old King’s Elementary on the first day of school. And I’m not talking about home schooling or distance learning. She can just take a year off. Or she can miss the first month or two until she’s cleared to be vaccinated.
I’d prefer that she graduate a year late than never graduate at all.
This is all because of the cult of orange.
Even though their orange messiah was secretly vaccinated in January, they still think that not taking the shot, and by extension reigniting the pandemic, killing Americans, and destroying a recovering economy, that they’re somehow owning the libs.
It’s pathetic.
Pat says
I support your difficult decision. Protecting your child is utmost.it is a shame our Board of Education has an antivaxer and others that are being controlled by our governor. Wishing you the best for you and your child
Deborah Coffey says
I feel your frustration. As a retired teacher, mother of two, grandmother and great grandmother, I’m pretty sure I would have made the same decision. Where the hell is the leadership in Flagler and Florida? However, it is never too late to be learning. Your daughter will be fine educationally and best of all, she will be safe.
Redfish Dave says
The present outbreak most likely began as a result of the ‘mask free mingling’ we were encouraged to do over the 4th of July weekend. God help us all!
CF says
Nobody ever advocated for unvaccinated people to “mask free mingle”. People that did that were well aware that should not be. They either did not care, or ignored that advice.
Deborah Coffey says
No. We can’t afford any more misinformation on Covid. Get the facts, please. We are in this predicament precisely because millions of people refused to get the vaccine.
Mod says
To those who don’t know this
The governor has veto power over the department of health
It all comes down to desantis… the buck stop with him
Remember that
Pat says
I never thought I would reach a point of apathy. People who are not vaccinated and become sick, deserve to suffer consequences of their choice.
I am vaccinated and I wear a mask. I am tired of those that say it is their choice to not get vaccinated.
I am tired of having to change my life for their choices and live In Fear of a new mutation to which my vaccination may no longer be effective.
Shame too on our Governor that denies the current situation. Does he not realize the economy will rebound once this pandemic passes. Do what is needed to stop it now.
Disgusted PC Resident says
I agree. I know people who died before there was a vaccine, people in their 30s who are long-haulers. I personally know people in other countries begging for the vaccine while the idiots here have to be bribed to get it and still won’t.
Unless you are one of the VERY FEW who medically cannot get the vaccine. SHAME ON YOU! You don’t want to get the vaccine, then you should be the one who has to stay the hell home. Sign a waiver saying you didn’t get the vaccine, don’t believe in science, and don’t want medical care if/when you get sick. Clean the gene pool a bit.
I’ve never felt this Darwinian in my lie, but I’m sick of losing the second year of my life having to stay home because of the irresponsible behavior of others.
Deborah Coffey says
Ditto.
Random says
I had COVID 2 years ago when it first broke out, I still cannot get the vaccine due to the fact I had the antibodies already, but no certification I’m safe or anything either as the Vaccine does less of protection (proven by people getting it while vaccinated) than anyone I know who’s got the antibodies naturally. I cannot be a risk as I cannot get it because of the antibodies I have in my system, proven over the 2 years since and everyone I’ve been around has yet to get it. Also masks only make sense if you’re around people for long periods, going in and out of a Circle K isn’t a mask need, stated by the CDC that it’s 15 minutes of being in contact that you’re at risk.
Kelley says
This is just sad and disgusting, what the current GOP has done to the party is horrific, I’m an independent and just don’t understand it. I’ve probably voted for more republicans over my lifetime than democrats but not anymore.
Jimbo99 says
Not much you can do beyond living your life and hoping for the best. We saw what happens shutting the economy down. Domestic violence increases, people are financially ruined, people still die from it. But hey, we got plenty of money for a splash pad & pickleball courts.
So a 4th wave of the virus, Delta variant(s), and Biden-Harris are going to end Covid relief ? Go figure that ? BTW, this is being linked back to the July 4th super spreader events ? By Monday, August 2021 is here, how come deaths are stuck at 114 still in Flagler county, like they have since the beginning of May 2021 ? Don’t get me wrong, I’m not for anyone dying from this, but it has been 3+ weeks since July 4th, nearly 90 days since the beginning of May. This doesn’t add up when the Delta variant(s) are touted to be more infectious & stronger than prior Covid strains. Someone is spinning misinformation with only case counts and no deaths. Especially, when it’s being reported that virtually every new case are the unvaccinated ? No vaccinations, no immunity among the new cases, you would expect a higher mortality rate for the Delta variant(s) that are the strongest yet ?
Another One Lost says
The delta variant is sweeping through Flagler county. The hospital ER’s are being overwhelmed with new Covid patients. The number of new infections is skyrocketing! Fox news tells me not to worry. CNN tell me that the end is near. In the mean time here at home there is an interesting oxymoron unfolding. No one is DYING from the DEADLY delta variant. The answer may be that I’m using the wrong metric. Conservatives look to mortality rates while liberals count the number of new infections. Conservatives hate liberals. Liberals dismiss conservatives as mindless “Trumpers”. I agree that the end may very well be near. Ironically it has nothing to do with Covid.
Disgusted PC Resident says
People not only die OF Covid, they die BECAUSE of Covid.
My neighbor lost her mother because her surgery was postponed so many times because of Covid. No way is she the only one.
PCvoter says
If you are worried about financial ruin rather than your health, think about this. A woman, whose husband died in the hospital with Covid, received a hospital bill for six million dollars. She was told not to worry about it as the government or insurance would pick up the tab. Now multiply that $6 mil times all the hospitalized Covid sufferers. That’s what I call financial ruin. My thoughts are that if you refuse to get vaccinated you should pay your own hospital bill and not receive social security disability benefits for long haulers. You should be locked out of all stores, bars, restaurants and any public facility so that responsible, vaccinated people can go out (with masks) without fear of getting infected by dumbasses like you.
Kat says
I see a lot of emotions here and I have to say at this point I am getting very angry. I work in healthcare and I take care of extremely vulnerable immunocompromised people, some of whom cannot get the vaccine. I have patients in the ICU right now who couldn’t get vaccinated for valid medical reasons and are battling Covid.
I ran errands in several places around Flagler county on Tuesday and in multiple instances, I was the only person inside a store that had on a mask. I have been fully vaccinated since January, I am wearing a mask to protect not only myself, but other people in my community- the same people who don’t have the common courtesy to return the favor.
I have made a good faith, calm, and concentrated effort to have an open discussion with any one of my patients or their family members who are not vaccinated. Some of the stupidity I’ve encountered is beyond description. The other day I actually had somebody say to me that they didn’t believe they should’ve gotten the polio vaccine because “Who knows what kind of affects that may have had on people”. I pointed out to them that the effects of the polio vaccine are absolutely clearly known- IT WORKED AND NOW WE DON’T HAVE POLIO! Guess what? The vaccines for diphtheria, tetanus, pertussis, mumps, measles, rubella and hepatitis work too! Thank God our “greatest generation” rolled up their sleeves and did what’s best for the common good (literally and figuratively, in more ways than one) and didn’t act like a bunch of self-serving, whiny, spoiled children – unlike 50.8% of the current US population.
To anybody reading this who is unvaccinated, I don’t care anymore if you personally get sick. I do care if you make other people sick and I do care if you become a drain on society. I care about the toll this is taking on our healthcare workers, the same people that you regarded as heroes when the pandemic first started and now you’re back to taking for granted again. I care about our teachers and children who are not old enough to get the vaccine, remember when you had to teach your own kids and you realized what a hard job that really was? I am angry because your selfishness and stupidity our crippling our community, negatively affecting our economy, and robbing people of experiences with their family and friends.
Many of the same people who rally against their perceived personal freedoms being up infringed upon are the same people that rally against anything they deem to be a “socialist program”. Well let me tell you, Medicare, Medicaid, and Social Security disability are all “socialist programs”. Police, fire, EMS personnel and the roads they travel on to get to your house to transport your sick, sorry self to the hospital are socially funded. Your ass doesn’t deserve a ride in an ambulance, or any of my taxpayer dollars going for your care during or after your illness. How many long haul Covid patients are going to wind up on Social Security disability? They’ll have no problem putting their hand out for a socialist favor then, will they?
Rant over, and if somebody has already pointed out, I can’t fix stupid.
Ray W. says
Thank you for your urgent and concise message. Something tells me that you really do still care for anyone who gets sick, though your expressions of anger and frustration is palpable throughout your comment.
A Concerned Observer says
I fully agree with this commenter. People keep coming up with their personal (albeit indefensible) reasons for not being vaccinated. They are totally intractable, selfish people that will not change their mind until they find themselves or their family in a COVID ward connected to several machines and surrounded be medical personnel desperately trying to save their lives. They are in unrelenting pain, have great difficulty breathing and are suddenly terrified to realize that they or their loved ones may die from this illness. We’ve all heard from them during nightly TV news reports how badly they wish they got the shot. We must come up with a method to place the burden of their inaction, which affects them directly, and not punish rest of society suffering from the continued spreading of this scourge.
Here’s a refreshingly new approach that just might work. Rather than providing “A Carrot” of cash payments and other gifts or perks (which are ultimately funded by taxpayers) to convince them to get vaccinated, how about “A Stick” whereby their Medicare or insurance carrier is not responsible to cover any COVID related medical bills? The cost of COVID treatment can very well run into millions of dollars of debt for them and their families not because of actual medical reasons or being ineligible for the prevailing vaccine, but just because they simply chose not to get vaccinated. This caveat could also extend to their immediate family that comes down with the same strain of COVID from living in close proximity to them. Give them a simple reason to get vaccinated which they can understand.
Disgusted PC Resident says
I agree with every word you wrote.
This situation has broken me. I have done everything right, but I’m the one on house arrest because of the selfish bastards who won’t get vaccinated.
As I said, I feel broken. I spent some time with a good friend — both of us sitting in our cars in a parking lot — consoling each other. I hope you have someone like that.
T says
Argee thank you for service and knowledge most don’t have that.
Concerned Citizen says
You know all the rants about freedom would be so funny if the cost wasn’t so deadly.
I got my shot as soon as I was eligible for it. I have a wife in the healthcare field. And I have parents in their 70’s and 80’s. My stepfather got it in the early phases and it nearly killed him. He’s still recovering. My wife?She’s on the front lines dealing with it for days.I wear the mask and got the shot because it’s the right thing to do. And you know what? After serving my country for the better part of 16 years and a career in Public Safety I don’t feel the least bit oppressed over having to wear a simple cloth covering when out and about. Hell I had more shots than you can imagine my first week of Basic in the Airforce.
Our country has become one of the most selfish on this planet. Other places have mask mandates. Other places are considering vaccine mandates. Our government even with the mixed messages tried to go lienient on us. And issue guidelines. Not mandates. my goodness you all would flip when they mandate things.
I said it in posts long ago. Personal beliefs aside and party affiliations regardless. The longer we take to do the right thing. And flatten this the longer we have to deal with it.
John says
[Do not use this site to spread disinformation. Thanks.–FL]
If you already had covid you don’t need the vaccine for you have antibodies. I have had covid and have no issues. 99.8 percent chance of survival. I am tired of the lies that come from our leader in the white house. Science says even if you had your vaccine you can catch it and spread it that’s why they’re telling you to mask up. And if you think antibodies don’t protect you then you have no clue how a vaccine works. This is why they report cases not death’s to scare more people to take the experimental vaccine. Look it up yourself on the FDA website approved for emergency experimental use. In the UK 60 percent of the people hospitalized had been vaccinated. Do some research before you criticize anyone. The last I heard this is still America
Greg says
Go to the Michael Yeadon interview on Bitchute and find out for yourself why there is such vaccine hesitancy.
He is a former Vice President for Pfizer.
A.j says
Blame blame, the Fla. Puppet Gov. That does not help us. We are responsible for our lives and the life of our family. Do what u need to do to protect your self. People continue to vote Repubs. Look at the result of them doing little to nothing for the people. People will put a lot of them in office next year. Just look at the recent special election in P. C. Take care of yourself, the Repubs & the Dems are taking of themselves. Look at crooked Trump & Puppet DeSantis. Just saying.
David Schaefer says
I just wish that people will wake up. This crap is real its not a joke vote these ahole republicans out of office PLEASE…
Only Me says
I don’t give a crap if you are Republican or Democrat start being responsbile and listen to the Doctors and Medical people or we will all be dead and then what have we accomplished NOTHING.
As far as all those in political positions you took and oath to protect and serve so start doing it and put your other crap aside.
Wake up people before businesses, grocery stores, everything starts shutting down because of this outbreak once again because those that think they are stronger and smarter didn’t listen to the professionals warning everyone what is going on.
I have never witnessed such a war of humanity going on in our country now, I can only imagine what the younger children are thinking right now about all of us that are disagreeing with how to save lives. And those that don’t want to get a vaccine or wear a mask you are committing basically murder on those you know and those you don’t know. Stop being so stubborn and do what is right for humanity. Be a hero in our lives and not our enemies.
David Schaefer says
Last night a poll came out a good source said that it’s white republicans were at the top of the list who refused the vaccine.
really says
really, I don’t care red or blue it is up the induvial to get vaccinated. let’s not place blame on the fl gov nor the us president. btw Orange and Osceola county are on fire with covid right now and it is purely a democratic majority. place the blame where it belongs on the unvaccinated. I’m tired of enabling the unvaxed – I got my shot and not going to wear a mask because you refuse to do the same. no longer my problem. maybe pelosi got it wrong – don’t arrest those without a mask in public arrest those unvaccinated without a mask in public.
stop helping those who want no help
Jane says
Don’t go to Walmart without a mask please!!! Protect yourself and your neighbors !
really says
[Do not use this site to spread disinformation. Your reference to having more chances of getting shot or hit by a car is false. Thanks.–FL]
protect myself from what if I’m vaccinated? The chance of being vaccinated and getting a serious health problem due to covid is negligible _ I’d have a better chance of getting shot or hit by a car walking into walmart. if my neighbor is not vaccinated then they should stay in their home and avoid the public
oldtimer says
This may only be a small part of the problem but I find it interesting that everyone talks about the people who refuse to get the shot no one mentions the THOUSANDS of people coming over the border that our own government is transporting all over the country. No one is taking into account that more than a few of these people are covid positive,but hey don’t worry all is well according to the VP
David Schaefer says
That’s coming out of the mouths of stupid people look at the current map Florida for example…..
Steve says
oh boy WHATABOUTISM out of the orange blowhards play book page 4
oldtimer says
First, I’m not a trumper, second I got a shot. It’s a legitimate question ..the same president who is telling us all to get the shot is letting thousands of unvetted people into this country, how is that sane in any universe?
mark101 says
ITs not just our county, tke Lake and Sumter. 2 days ago. Advents Health Dr. Victor Herrera, AdventHealth Orlando’s chief medical officer, said nearly all COVID-19 patients in hospitals are unvaccinated. ” “Over 90 percent of patients that are in the hospital right now with COVID-19 did not get a COVID-19 vaccine.”
I don’t care what party you belong to, get vaccinated. Hell the life you save or your future health might be your own.
Sean Cononie says
Hi, we run the Homeless Voice Covid-19 Response and Vaccination team. It was RV in the parking lot in this story. We will be in this area in the next week or two trying to get to the hard-to-reach homeless population their vaccines. We hope people will change their minds and get their shots. It is our job at this point in time.
FlaglerLive says
Thank you for that clarification.
Sherry says
As a person who gets daily cancer treatments at Palm Coast Advent hospital, I am astonished at how many of their medical staff have NOT been vaccinated. I ask every staff member who comes near me if they’ve been vaccinated and so far about 40% say “NO” or refuse to answer. If they have NOT been vaccinated, I politely ask for a staff member who is. I’ve even gotten very confrontive push back from a PA when I asked if my chart could be notated that I require only vaccinated staff members to treat me.
I’ve been told that generally patients do NOT ask about vaccine status and therefore staff does like such questions.
My best advice to you all is to take personal responsibility for your health care. Do NOT assume that medical professionals are vaccinated. ASK questions and protect yourself from “UN-NECESSARY” pain and suffering, even when being treated in a hospital.
David Schaefer says
Go up to mayo clinic you will find a different situation up there. I worked in the OR in 2 different states and was tested for infectious diseases all the time. My opinion is everyone who works in the medical field needs to get the vaccine or be tested 2 times weekly or go lose their job period………….
J. Michael Kelley says
Reading the comments leaves me wondering what have we become. For those that blame “Republicans” why would they be antivax when the vaccine was developed under the Trump administration. “Republicans, as has been so eloquently described, think highly of the past President, so they should be energized to get the experimental gene therapy medication. Then Republicans say very negative statements about “Democrats”, after all they are all Socialists. We as a people better stop all this nonsense, and recognize the destruction it is causing.
Dan says
All the people arguing about Republican this or Democrat that, Both parties are using the covid epidemic as a means to garner more political power. People that come with politics & insults first are not doing anyone any favors. More of a simple minded approach to a problem. This tribalism will not lead to a better future for either side. Its actually pretty sad that we have become so divided by political affiliation.