A 68-year-old woman was confirmed to have died of Covid-19 on Friday, and another 68-year-old woman was confirmed to have died of the disease today, according to the latest Florida Department of Health data, bringing Flagler County’s total number of deaths attributed to the coronavirus to four.
Previously, a 77-year-old man died on March 26, and a 72-year-old woman died on March 22. While both the earlier patients had had contact with others who’d been exposed to the virus, the department could not confirm any such contact with the two latest victims, underscoring the extent of so-called community transmission–meaning that the virus had been propagating in the community.
The deaths add to a statewide tally approaching 1,500 as the Institute for Health Metrics and Evaluation, one of the models most closely watched by state and federal officials, revised significantly upward its estimate of deaths for Florida, to nearly 4,000, by August 4, with a curve descending at a much slower rate than previously calculated.
“The social distancing and restricting public gatherings is one of the many injects into that model,” Flagler County Emergency Management Chief Jonathan Lord, who monitors the model, said. “So when you start phasing out social distancing anywhere in the country, you can now see that there’s an impact with the reopening of America.”
The institute’s projections echo a somewhat more dire report by the Centers for Disease Control that forecasts 200,000 new Covid-19 cases a day by the end of May, up from 30,000 new cases at the moment, and 3,000 deaths per day by June 1, nationwide.
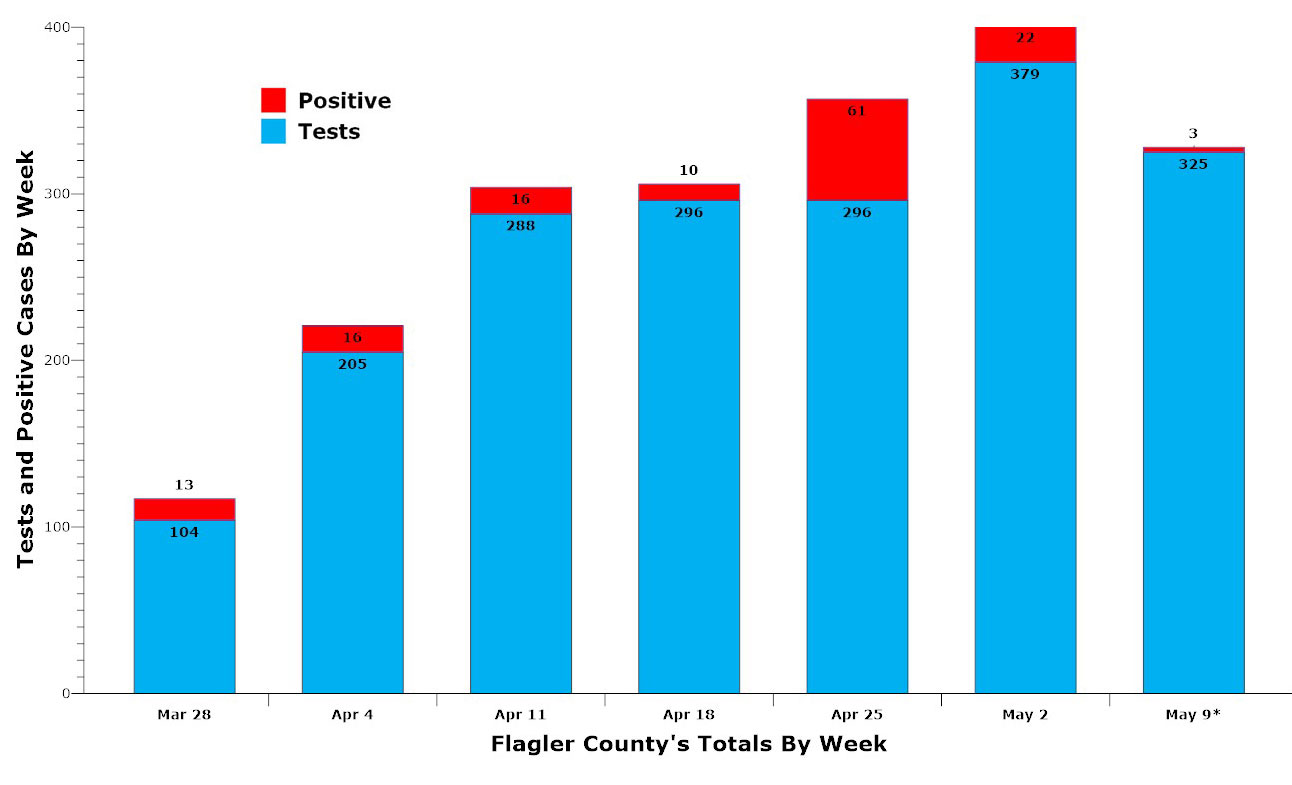
But the CDC reports sees different areas affected very differently. It sees Flagler County for example, in the category of “sustained decline” of new cases. That decline is illustrated by the last two week’s testing numbers, which show a smaller proportion of positive cases relative to the number of tests: 6 percent last week, barely 1 percent in three days of reported testing numbers so far this week. But Lord and Dr. Stephen Bickel, the medical director for the health department in Flagler and Volusia, caution that one of the reason the ratio is lower is because testing criteria is much broader. Previously, only people with a list of Covid-like symptoms were being tested, which increased the possibility of positive results. Now, the testing at the drive-up site, on the campus of Daytona State College, is open to anyone with any single flu-like symptom. That’s lowered the incidence of positive results.
Still, the downward trend, for now, is clear, if not nearly as pronounced as officials would like it to be. It’s a slow decline, and it’s rife with caveats, among them, Lord says, the fact that any single week’s numbers can be deceptive. It’s the accumulation of weeks that matters.
Raising slight alarms, too, are indications in the latest Department of Health figures of an uptick in local emergency room visits of people with influenza-like illnesses, and with Covid-like illnesses. Specifically, those reporting Covid-like illnesses had numbered 50 the week ending March 22. The numbers dropped steadily to 20 each of the weeks ending April 12 and 19, but have then risen back to nearly 40 the week ending April 26. Again, a single week’s upswing or downswing does not make a trend. And AdventHealth Palm Coast’s bed count has plenty of capacity, according to numbers released by the state Agency for Health Care Administration.
All those indicators are playing in Flagler’s favor, and are reflected in many other counties across the state. Notably, the CDC report also sees sustained decline of Covid-19 cases in South Florida, the areas most severely struck by Covid-19 in Florida in spring. But counties along the I-4 corridor and the Tampa Bay region would experience either an “elevated incidence plateau” or actual elevated growth in new cases–as would most counties in Georgia, which has taken more aggressive steps to reopen.
“There remains a large number of counties whose burden continues to grow or are in elevated incidence plateau,” the CDC report states, “including the Great Lakes region, parts of the Southeast, Northeast, and around southern California.”
Lord cautions that the models are calculated with a constant new flow of data, and that Florida’s projections are likely to reflect the fact that while a reopening is taking place, Gov. Ron DeSantis is applying it in much more cautious steps than Georgia, “basically opened the floodgates.” If Florida’s governor stays the course, Lord said, the models should reflect the change. “I would love to see that the predictions don’t come true,” he said, but along those lines, it has to do with residents’ and businesses’ behaviors and staying within the boundaries the governor sets.
Dr. Stephen Bickel, the medical director at the Flagler and Volusia health departments, who analyzes reams of Covid-19 monographs, articles and data, sets out five criteria for a community to reopen confidently, and grades each when applying it to Flagler. First, the data must show a clear trend in the county’;s favor, in terms of declining positive cases and percent of positive cases versus testing overall. He gives that criteria only half a point. Second, there must be adequate testing. With Flagler ramping up testing somewhat, but not massively–the number of tests reached 379 last week, the highest single-week total since the coronavirus emergency began–he gives that half a point as well.
Third, there must be a surge of a public health contingent to carry out all the contact tracing, containment and monitoring necessary. He gives that no points, because while there are some 30 people fulfilling that role locally, it’s not where it must be The fourth and fifth criteria are ensuring that health care workers have enough personal protective equipment, and ensuring that there are enough hospital resources to handle a surge. He gives each a full point. Totaling it up, “I give it three points out of five,” Bickel said. “It’s not enough.”
Bickel said the local health department, within its means, is trying to do what should be done statewide and nationally: push for as much testing as possible and contact-trace and monitor on a systematic basis. But the resources are still lacking, a victim of national and state policies that have not been in sync, allowing for a patchwork approach that defies the unified front required in the face of a pandemic that respects no borders, and that will affect every community in time. “It’s all this disjointed approach that’s just kind of like asking for trouble,” Bickel said.
He recognizes the debate about reopening the nation economically, and balancing that with the risk of more deaths. But he sees that as a false and dangerous dichotomy: it’s not either or. It doesn’t have to be the economy or the fatalities. “There is a third way,” he said. That third way is to invest in an army of public health workers and technology to monitor the flares or extent of any Covid-19 incidence in every community, the way Taiwan, Hong Kong and South Korea have, thus enabling public health departments to immediately know who is infected and where the clusters are. With armies of contact tracers, infections can be detected, infected persons isolated, and society allowed to go on about its business, as has been the case in Southeast Asia. It would take billions, possibly hundreds of billions of dollars to get to that point, Bickel acknowledges–but it would still be far less expensive to American society than the trillions being spent on relief to businesses and individuals, while the nation hobbles toward a depression.
“I think the state could pull it off even if nationally they did not,” Bickel said. But from the start, the national approach has been flawed, scuttling efforts down the line. “We dropped the ball on the testing big time, we never came up with a strategy to rectify that, and we should have known it would have been a challenge to open up. Anybody who doesn’t think it’s going to be a challenge doesn’t understand what’s going on right now.”
.

























HappyHappyJoyJoy says
Based on reporting from the Palm Beach Post, at least 171 people in 40 counties had COVID symptoms, some as early as Jan 1st. They have all tested positive and at least 103 did NOT have any travel history. The remainder had traveled but none traveled to China. Pot meet kettle—your country of origin, is not China.
The earliest cases in two countries have the “A” strain, which is the strain most closely linked to the original found in bats. Those countries are USA and Australia. The research is pretty damning, actually. Search for some of the peer reviewed reports that show Wuhan has primarily the “B” strain, which is a mutation of the original “A.” Wuhan scientists and Australian scientists worked on coronaviruses from the bats with a 96% genetic match to this current COVID outside of China. They worked in this in Australia. Australia, in the spring of 2019 had the worst flu season in record with an abnormally high number of pneumonia cases. The US freaked and pushed everyone to get their flu shots harder than usual. Why? Not to protect them from the flu, per se, but to see how many flu-like illnesses presented with pneumonia that had a negative flu test. How many people in the US from October (some of the earliest recorded cases are from Nov 5, which means infection happened in Oct) until now died from this and it was called pneumonia, heart attack, stroke, etc.
Something is WAY off here. I’m not saying intentional by any means but once again, as history shows, we are not being told the truth. I don’t care what the test rate is in Palm Coast, we need to know the rate of antibodies. I am more convinced than ever I had this in March and I STILL continue to have symptoms off and on and it’s May. It’s like The Walking Dead (spoiler alert—stop now—you’ve been warned—last chance)—we are all infected.
joe says
https://www.palmbeachpost.com/news/20200505/coronavirus-florida-patients-in-florida-had-symptoms-as-early-as-january
“Florida on Monday night removed data from the Department of Health website that showed 171 patients had coronavirus symptoms or positive test results in January and February, before any cases were announced to the public.” (From the article)
Florida has a Trump wanna-be as a Governor – evaluate accordingly.
jake says
Nonsense, “COVID-19 was first confirmed in Australia in late January 2020. This page provides a number of visual representations of information about COVID-19 in Australia since that time.”
https://www.health.gov.au/news/health-alerts/novel-coronavirus-2019-ncov-health-alert/coronavirus-covid-19-current-situation-and-case-numbers
TeddyBallGame says
Ergo: If you are 65 or older AND/OR have and underlying aggravating condition you need to keep sheltering in place. Worldwide, 90 to 95% of all deaths so far are within this population. If you are not in this subset you still need to observe reasonable social distance AND ware a mask when in an indoor public space.
If everybody does these two simple things, many of your fellow citizens lives will be saved and the sooner this thing will be behind us.
What to do about multigenerational households is a BIG problem.
Infected or Not says
I was tested last Wednesday and still have not received my results. Many people have been waiting for their results online, some had waited up to three weeks. When we call AdventHealth and ask why the results aren’t in yet, we get transferred to a “Recorded Line” that tells us “Due to a high volume of tests, results are going to take a while”. I doubt many people got their results from last weeks “Mobile Testing Site” at Daytona State. I need my results so I can return to work. (102 degree fever, fatigue, slight congestion were my symptoms)
Willy Boy says
It’a mutated. Need some 100 degree temps to slow this killer down.
Darksideofthemoon says
Models?? If we believed these models we would bury ourselves before we even became ill. 6 people per 100000 died- majority over 70- majority in southern counties- and yet the paranoia continues! It’s almost as if people lost the ability to reason for themselves.
Well... says
@HHJJ Very interesting article. Makes you think just how long has this really been here, spreading, masquerading as the “flu,” at least based on symptomatology. I’m sure we are not being told even 5% of the truth. We never are…it’s how the world works, sadly. I do agree that antibody testing (regardless of what it means) is a critical step in opening up the county. Perhaps that’s why the numbers are waning, people had this and are still feeling the effects but don’t have enough of the viral load to test positive. Roache developed a test that will 100% tell you if you NEVER had the virus. The positivity rate is around 99.6% but the negative rate is 100% so it is important places use this test rather than some of the junk ones that flooded the market. The Navy also uses a very accurate test that gives results in about 15 min. They are willing to allow mass production of this antibody test kit as well, so that’s another one worth thinking about.
I too have a sneaking suspicion I had this as well in late February. I had my flu shot (not a 100% protector, I know) but whenever I get sick, I NEVER have shortness of breath. Ever. I’m 40 and I know what I’m like when I have the flu, or bronchitis, or a URI, and so on. In late February, I couldn’t walk from my cubicle at work to the bathroom without gasping for air. I thought, maybe I wasn’t breathing right, you know lost in thought daydreaming about moving to Iceland or something. But then it happened on my way back. It happened on my next trip. It happened when I went to the printer. One time, I almost passed out in the bathroom and fell against the stall wall. I knew I wasn’t getting enough oxygen, I could sense something was wrong. Yeah, I should’ve gone to the hospital. Shoulda, woulda, coulda, but I had obligations that prevented me from going, so I didn’t.
For roughly a month, I couldn’t take deep breaths. My chest hurt and ached. I was winded just walking into the kitchen to get more water. All I wanted to do was sleep. I couldn’t stay awake longer than a few hours at a time. I couldn’t touch the back of my neck it hurt so bad, with pain radiating upwards into my head, and toward my spine. I never had a headache as bad as I did and it lasted for three weeks, and I mean a stabbing pain that woke me up from sleep. It affected my vision, my personality, it affected my ability to find the words I wanted to say, I couldn’t remember conversations just had, and I would just sit many times, with an empty void in my head. That was very disconcerting to say the least. I had chills where I couldn’t get warm no matter how hard I tried. I wore three shirts, a thick hoodie, and used a winter blanket and I still shook. I lost my sense of smell and my sense of taste wasn’t as sharp. The bottoms of my feet hurt like someone was stabbing knives into them, sitting, standing, and walking. The sore throat lasted for three weeks, just a persistent ache. A dry cough. Gastric upset. Loss of appetite. Nausea. Achy body. I had so many symptoms of this, but couldn’t get a test either because I had no travel connection. I think that actually doomed places and led to a lot of unnecessary deaths. The strict set of criteria used to test people in the initial stages, when this obviously (as many reports circulating suggest) has been creeping across the world, maybe even as early as Oct/Nov in places. Many of the earliest cases they are finding have NO travel connection to China or connection to any known confirmed cases so who knows just how long this has been moving across the globe.
It is May 6th and I still have symptoms of this that come back with a vengeance, lasting for a few days, and then I’m better again. I haven’t left the house since March 20th, luckily I can work from home (I’m not sure I have enough energy to drive there and work the full day so, I’m very grateful for that option). In March, April, and just last week into this weekend, for 3-4 days each time, I had a fever, chills, sore throat, dry cough, malaise, mental confusion, and a sense that I am not getting enough oxygen. It’s not my allergies since I take a boatload of meds that do work. Am I still contagious? No clue. How long does this stay in someone’s system? No clue. As long as we have antibodies, will this flare up? No clue. Who know what this is or where it started and it really doesn’t matter, ’cause it happened, and it’s out there, and now humanity has to deal with it, probably for many, many years. What is important is knowledge and we need more of that and less secrecy.
WhackAMole says
Less than 2,000 people in Flagler County have been tested. Unreal. Let’s open back on up, right? 1918 will look like a walk in the park after this is over. Shameful.