Two staffers have tested positive for the coronavirus at two assisted living facilities in Palm Coast–one at Brookdale Palm Coast–Formerly Sterling House–and one at Princeton Village of Palm Coast, according to figures released by the Florida Department of Health. They are the first two cases affecting local long-term care facilities, where authorities have been especially vigilant in attempts to prevent infections of a disease that preys especially on the elderly.
The cases are among a total of 127 Covid-19 cases so far reported in Flagler since the beginning of the emergency in mid-March, with 10 hospitalizations. Both numbers are cumulative, meaning that they still include the number of people who have recovered, or been discharged from hospital (two have died). Florida crossed the 1,000-deaths threshold over the weekend, with deaths in the state at 1,088 today, and past 50,000 in the nation. In Florida, people 65 or older account for 83 percent of deaths
In other developments, the Flagler Health Department expects to be among the recipients of the first batch of rapid antibody tests that the state will be distributing to counties in early May, but the tests will be limited primarily to health care workers, and the health department’s medical director cautions against seeing a panacea in the tests.
The county’s Covid-19 testing site at Daytona State College is not operating today or tomorrow, but will resume testing Wednesday in an expanded partnership with AdventHealth Palm Coast, and will expand criteria: testing will be available to anyone who has symptoms or anyone who has had close contact with someone who tested positive for COVID-19, even if they are not currently experiencing symptoms, according to a county release. Those who wish to be tested do not need a doctor’s order. Those interested in being tested are to register at AdventHealthCoronaVirusTesting.com or by calling 877-Virus-HQ (877-847-8747).
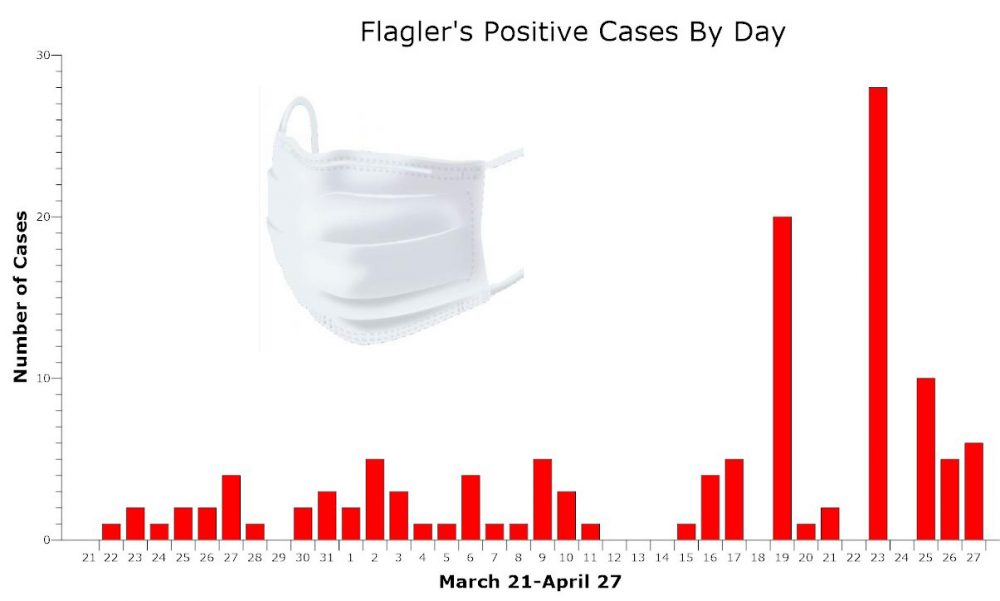
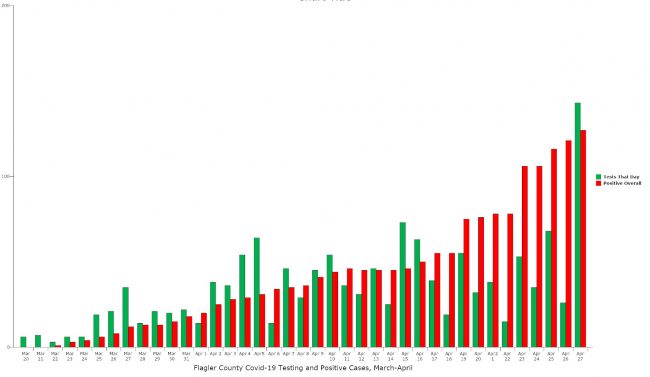
While the county and Flagler Breach have reopened beaches for 24 hour use, as long as it is limited to exercise rather than socializing (a directive that’s not always followed rigorously), local officials have been keeping an eye on a curve of positive cases that’s not yet flattening in Flagler, even though testing has not increased significantly. There were 319 tests three weeks ago, 320 two weeks ago, and 267 last week, overall, according to Department of Health figures. The department’s figures lag behind somewhat: this morning’s report indicates 143 additional tests, a reflection of the testing conducted at the DSC site, where testing has confirmed many of the positive cases.
“For us locally in Flagler the number was a 9 percent positivity rate, so I don’t see it going down yet for Flagler,” Snyder said. In fact, the positivity rate has inched up from 7 percent early last week. “But the positivity rate statewide for just new cases is 6 percent, so that’s a real plus. It basically tells us–again, keeping in mind it’s just the new cases–it’s a positive trend downward. But here in Flagler because we are ramping up testing locally with the site at the college, we’re still two weeks into it, we’re still seeing positive cases.” The site produced 10 positive cases out of 43 tests in one day last week, then 23 out of 79 tests, then 10 out of 43. On Thursday, it produced five positive results out of 82. “One day does not a trend make, but you can see how it’s still going up and down, up and down,” Snyder said. “We’re going to learn a lot over the next two weeks.” He projects a downward trend.
Across Florida, 1,140 residents of long-term care facilities have tested positive for Covid-19, out of 147,500 residents (an infection rate of 0.8 percent), and 1,074 staffers have tested positive, out of 195,000 staffers, for an infection rate of 0.6 percent, and 319 residents or staffers at long-term care facilities have died of the disease, according to the health department.
There are 71 long-term care facilities in Palm Coast and Flagler, including larger assisted living facilities and nursing homes as well as smaller group homes for adults or for adults with disabilities–typically residential homes with four to six residents each. Brookdale and Princeton are among the larger facilities.
The Flagler County Health Department’s staffers have been fanning out to the 71 facilities since last week to ensure compliance with safety guidelines. “I decided early last week that now would be a good time to just put into higher priority visiting them and not just relying on phone calls, but actually eyeballing, observing, meeting with their management teams, meeting with the owners of the homes,” Flagler Health Department Chief Bob Snyder said today. The visits entail walk-throughs with checklists in hand that ensure health department and Agency for Health Care Administration guidelines are followed.
“We have not experienced a any significant issues in doing this review, this fac to face review,” Snyder said. “We did run across one small operation that needed more PPE supplies,” meaning personal protection equipment, “so we are following through on that, that’s specifically gloves and masks, so it was good that we visited that place.”
When a long-term care facility staffer tests positive, the staffer is required to self-quarantine at home for 14 days. The staffer is allowed back at work only after getting two negative tests for Covid-19, separated by 96 hours. Meanwhile, some of the health department’s 26-member team of contact tracers and epidemiologists go to work, tracking back all the infected individual’s contacts at the facility and elsewhere. All the health workers who have had contact with the person are contacted, all the people at work or at home who have had prolonged contact with the infected person are asked to self-isolate and monitor their symptoms in tandem with health department tracers, who check on them by phone daily. The tracers also check for symptoms among contacts.
If a resident of an assisted living facility tests positive, the resident is isolated. “There is a place in each facility designated as a place where positive individuals would be cohorted, in a private room,” Snyder said, with staffers appropriately trained to take care of the patient.
Snyder said there has not been an exodus of residents from facilities in Flagler and Palm Coast. It is one of the trends the department checks on. “I have heard of that happening in other larger communities, but not here, thankfully,” he said.
Snyder today said antibody tests are on the way, from two of the four companies approved by the Food and Drug Administration.
But he and Dr. Stephen Bickel, the medical director at the Flagler and Volusia health departments, downplayed the focus on the antibody tests as any sort of panacea. The tests will have their uses, they say, but those uses must be understood in the context of the tests’ accuracy and the tests’ subjects: testing health workers, who are at higher risk of infection, is not the same as testing the population at large, where the risk is lower. The difference may point to the validity of the tests in some cases, their invalidity in others.
Antibody testing, also called serology testing, is a quick finger-prick-like blood test designed to detect whether the body has developed antibodies to fight infection. If the antibodies are detected, it means the person built up defenses, and was therefore infected in the past, though it is also possible that the person is still infected. (Doctors can pick out two types of antibodies, one that’s developed early in an infection, and one that develops post-recovery. But researchers still don’t know how long it takes for the second kind to develop after a Covid-19 infection.)
Antibody testing is not a test for the virus. Researchers still do not know how long antibodies protect against the virus, but the hope is that antibodies point to a measure of immunity.
As with Covid-19 testing, antibody testing has also been facing obstacles: not enough tests, and flawed tests. If the tests can’t be trusted, then the results are useless because they’d still amount to gambling. Few companies have produced reliable tests. Most have not, making them unreliable–for now–as guideposts for policy.
Two factors determine a test’s accuracy: “specificity” is a test’s ability to correctly identify the absence of what’s being tested for–in this case, antibodies. If, for example, a test is 97 percent accurate, then its specificity is high. Sensitivity is the test’s ability to render a true positive rate. (Snyder said the tests Florida will be distributing “are valid, where the specificity and sensitivity levels are acceptable.” But keep in mind: the state recently recalled previously approved Covid-19 tests that the Centers for Disease Control had approved, and that proved flawed.)
In the population at large, where Covid-19 has been less prevalent than, say, among health workers with regular exposure to Covid-19 patients, an antibody tests that shows positive for antibodies in 4 percent of the population could have 3 percent of false positives, even with a highly accurate test. “So you’re overstating the prevalence of the condition,” and by a very large percentage, Bickel said. Put another way, if community testing was conducted through survey methods that took a sample of the population that resulted with a 3 percent false-positive rate, and the number was extrapolated to apply to Flagler’s population of 100,000 people who are adolescent or older, that would yield 3,000 false positives, compared to the rate currently shown by testing–less than 1 percent, thus rendering the antibody test essentially useless.
The same approach doesn’t apply with a group of health workers or people who have been screened for symptoms, among whom the positive rate has been closer to 10 percent: the proportion of false positives relative to their number would be much lower, making the test more useful.
In sum, Bickel said, it’s a misconception to rely on existing antibody tests as a true measure of the extent of past infections in a community, and it’s a waste of energy to test people who have already tested positive for the virus. “Use it to answer certain questions. But the surveillance I think is going to turn out to be a false hope–until the numbers get really higher,” he said.
The more pragmatic and reliable approach today is testing for Covid-19 on a massive scale. Bickel wants to see 1,000 tests a week in Flagler, week after week, as a means of keeping control of the disease and giving authorities a clearer picture of when and where it may be reemerging. “The virus testing is much more useful, you’re doing tons of it, you’re doing every week, you’re looking at the numbers it gives you a clearer picture of how this thing is moving along,” he said. Antibody testing won’t do that.
Bickel is not thrilled about last week’s number of positive cases, even though overall the county has done well to keep its numbers well below those originally feared. “We could be really risking stuff here,” he said, referring to a too-swift resumption of social and economic activities. “Forty new cases in Flagler in the last week, that’s a fair number. I’d like to see it more like under 10, but the natives are getting restless. How long are you doing this and the economic impact is huge.”



























HappyHappyJoyJoy says
The numbers are lower than anticipated because when people were really sick in March and early April, there was no testing for the majority of us between 20-50 that didn’t meet the strict criteria necessary. Even though antibody testing isn’t 100% foolproof, it will indicate just how many of us that couldn’t get tested may carry the antibodies. Also, don’t forget the increase in average of pneumonia deaths in February and March not attributed to the flu but also not tested for COVID.
The two dozen or so Trump supporters out there on Flagler Beach the other day getting restless is not indicative of the majority that do not want to rush this. My employer CANNOT enforce social distancing, therefore they CANNOT even follow the CDC guidelines for six-feet distancing without allowing those of us that want to, to continue working from home.
1918–social distancing ended too soon. It came back with a vengeance and killed more people in the 2nd and 3rd waves than in the first. Everything happening today, mask defiance, protesting to open the economy, and so on happened then too and those people “lived” to regret it by having up to 3% of the global population die, most in the latter two waves. COVID isn’t just killing the “weak” or the “infirm,” it is attacking healthy people too, in different ways like sudden strokes or heart attacks because the body is attacking its own blood vessels. In Europe they are seeing kids now, coming in with an inflammatory disease similar to Toxic Shock Syndrome or Kawasaki Disease. COVID is smart and unlike anything anyone has seen before. It feels its way around your immune system and just because you survived the strain you contracted, there are 30 mutated strains documented, some mild, some severe, so this isn’t over, not by a long shot.
Algernon says
What kind of test is being given for COVID19 at DSC? Is it the invasive nasal swab which is reportedly painful or is it different and easier on the patient?
Name (required) says
As an example myself, it’s seems More people that didn’t meet the previously required parameters (over 65; pronounced fever, cough, etc) for testing before last week, are being tested more now. And it seems the rate of cases among those by percentage, is higher. This is where we find that there are positive cases wandering around with minimal or less severe symptoms, possibly asymptomatic altogether. Be vigilant folks. Some well populated areas of town use the same mere handful of stores to make their daily purchases. Just a thought. It’s not over yet. Soon, hopefully and sadly, not quite yet. Put the distractions aside and be sensible. Please. We’re almost there.
Deputy sheriff says
No where near a downswing ….. but let’s open up those beaches !
marty barrett says
Hard to imagine cases are on the rise locally. I mean, yeah, we are crowding the beaches, going to grocery stores without masks, and standing arm in arm in full throated rage on street corners yelling about being aggrieved; but on the other hand there is still prayer, the sun, and Chlorox. Why oh why?
tulip says
I have forgotten, but weren’t there a couple of events that DeSantis would not shut down somewhere around Easter (April 12) it’s been 2 weeks, so maybe our case numbers will rise because people attended those events and are now beginning to get sick? Just a thought
Rob Jr says
Why worry?
Florida has a population of 21,400,000 give or take.
Florida public health reports testing of 366,875.
That is 1 and 3/4 of a percent of the total population that has been tested, give or take.
Woo Hoo.
Open up the state.
Hey stop the lies tell truth says
It’s a damn shame how our governor is covering up all the facts about the true death toll why else would it not be reporting in our local news as well as Nation wide news 😡.
Lal says
I am surprised it’s only 2 staffers so far because many workers have 2 or 3 jobs to make ends meet so they bounce between nursing homes and ALFs.