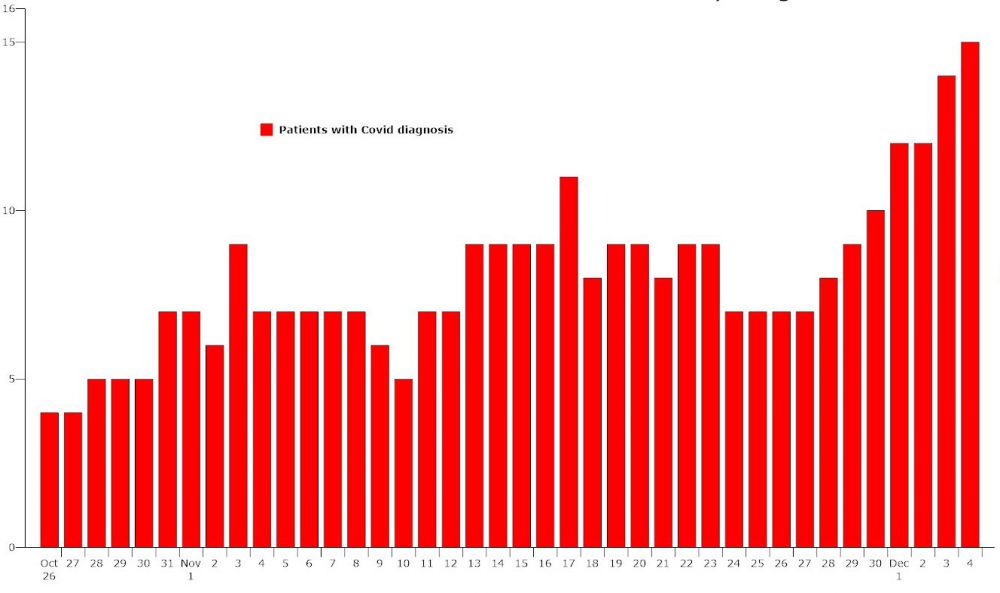
The Flagler County Health Department this week reported the 43rd covid-related death of a local resident, a 66-year-old white man, as covid-related hospitalizations at AdventHealth Palm Coast have ramped back up to levels last seen during the summer spike.
Hospitalizations at the local facility have increased almost daily, to 15 as of midday Friday, matching the number on Aug. 7. Hospitalizations have affected some 7 percent of people infected with the coronavirus in Flagler County–1 percent more than the state average–and 2 percent of those infected have died. According to the state Agency for Health Care Administration, 4,334 people are currently hospitalized with a primary diagnosis of Covid-19 across the state, including 109 in Volusia, 26 in St. Johns, and 2002 in Orange counties. It is not infrequent that patients from Flagler are cared for in surrounding counties, and vice versa.
Case loads in Flagler have again reached summer highs, with more than 150 cases a week for the last three weeks, though relative to other counties in the state, Flagler remains at the lower end of caseloads. Its latest seven-day average for daily cases, at 23.7, ranks it fourth-lowest among Florida’s 67 counties, and 67th-lowest since the beginning of the pandemic, strongly suggesting that the efforts of local public health and government officials, including mask mandates in all three cities, have been successful.
The same officials are stressing the importance of maintaining preventive measures such as mask-wearing, social distancing and frequent handwashing to ward off the more severe effects of the pandemic now cascading over the rest of the state and the nation.
“We do mirror what is happening out there,” Bob Snyder, who heads the Flagler County Health Department, said this morning. “Just two months ago, we were averaging 70 to 75 positive cases a week, and now we’re somewhere in the 160 to 175 range a week, positivity rate is 6.8 percent.”
The weekly count of emergency room visits by people complaining of Covid-like symptoms rose to above 40 in the week ending on Nov. 22, up from 25 the week of Oct. 25. “We are anticipating this to continue for a while, the next two to three months are going to be rough,” Snyder said.
Grim records are being set almost daily: On Dec. 3, almost 217,000 new cases were confirmed across the country, as were 2,857 deaths on that single day, close to the number of people killed on 9/11. The disease has claimed 276,375 lives in the nation so far, 18,873 in Florida, where just under 10,000 new cases were confirmed on Wednesday and 10,700 on Thursday, with 98 deaths. Florida’s seven-day average is 89 deaths per day.
After the school district recorded 32 new cases among students and staffers in each of the previous two weeks, numbers have fallen this week to a total of 10 cases, with the largest number–five–again at Flagler Palm Coast High School, whose principal, Tom Russell, has been hospitalized after testing positive for Cocid. He is in intensive care. Faculty at FPC are organizing morning prayers at the school’s flagpole at 7 a.m., before school hours begin. (“If teachers are electing to gather together at 7:00 a.m., outside of the work day (outside the school day),” Kristy Gavin, the school board attorney, said in an email, “this is permitted by DOE,” the Department of Education.)
Palm Coast Mayor Milissa Holland on Thursday said some 47 city employees are out either with a covid diagnosis, on quarantine because of contact with a covid individual, caring for an individual with covid, or out sick–almost double the number a week ago. Among those with a covid diagnosis is City Manager Matt Morton, who nevertheless took part in Tuesday’s City Council meeting by Zoom. The Palm Coast Fire Department had three individuals out two weeks ago, by they have returned, healthy, and the department is currently Covid-free.
In contrast, county officials continue not only to refuse to say how many of their employees are out or affected, but the county spokesperson and its human resources director have refused to say who is filling in for Joe King, the county’s acting fire chiefs, who has been out with a covid diagnosis since last week. (“When we have employees out for any reason, we have many qualified individuals that can step up,” Pamela Wu, the human resources director, said in an email by way of the county’s spokesperson.)
King took part in a weekly meeting with the Palm Coast and Flagler Beach fire chiefs around the time when he was being tested, but the meeting took place with broad social distancing, Palm Coast Fire Chief Jerry Forte said. Normally, Lenny Ensalaco, the interim deputy fire chief, would be in charge of the department in the chief’s absence. He also worked from home on Wednesday
At the county’s Emergency Management division, Jonathan Lord, who heads the division, has been working remotely for the past two weeks “out of an abundance of caution,” after possible exposure, though two tests have returned negative. “It’s about protecting my team,” he said. He will return on Monday. While three county commissioners attended meetings through the state association of counties earlier this week, newly-seated Commissioner Andy Dance was quarantined at home, with his wife Luci–an executive assistant in the administrative offices–through Friday.
Public health officials have been speaking of bringing the pandemic under control next year with the roll-out of the vaccine, but also warning of dangerous weeks and months in the interim.
Speaking on WNZF’s Free For All Fridays this morning, Snyder outlined in more details the coming roll-out. “We’re going to need a lot more people,” he said of staffing needs as the vaccine becomes available and, for a time, vaccination, covid testing and contact tracing will go on simultaneously. The vaccines will be distributed in multiple phases.
“Phase 1a is going to be health care workers and first responders, phase 1b will be people with high-risk conditions and those in long-term care facilities, nursing homes, and we’ll have Walgreens and CVS provide vaccines for those residents at our facilities,” Snyder said. “Then the second phase and third phase will be the largest. Second phase will be people who work in critical positions, people over the age of 65, with underlying conditions, correctional facilities, schools. Then phase three would be the big, big, general public, mass vaccination clinic concept. That could be through a drive-through or drop-off area, and drop-in, like at Cattleman’s Hall. We expect the first phase to last from the end of December ‘till about maybe the end of February, then come March, we should start seeing the larger phases occur, probably through the end of August, if everything goes well relative to this, logistically. So we’re ready. Moderna will follow Pfizer about a week later. So we’re expecting vaccines to arrive in about two weeks. They’ll ship directly to the hospitals, they’ll ship directly to the health department. So we’ll be coordinating with our community partners to get this accomplished. Can’t wait.”
![]()







Only Me says
Time for our City Officials make masks mandatory because Gov. DeSantis always will be ignoring all warnings of what is going on in the State of Florida which he took an oath of office to protect. And he wants to run for President, I don’t think that is a good idea when he can’t even protect the people that live in the State of Florida.
Before this gets out of hand our City and County Officials need to step up to the plate and do the right thing.
Percy's mother says
YOU are supposed to protect yourself . . . by wearing a mask at all times PROPERLY, social distancing, NOT going to unnecessary social gatherings where mask-wearing and social distancing is rarely practiced, and HAND WASHING.
Why do you expect Gov. DeSantis to protect you?
Aren’t you a semi-adult? OR, are you a child expecting to be taken care of by a parent figure?
Where is YOUR sense of responsibility?
Steve says
Hes the Governor and dropped the ball on his lack of response from the get go . He is failed leadership plain and simple with no plan. Just ignore and ride it out. He is a Science denier who needs to be Voted out like his Master on the Hill
The Truth says
I’m not worried about my sense of responsibility, I’m worried about the people who blindly follow Trump and DeSantis and don’t act in the well being of others.
The truth is, a mask mandate shouldn’t be necessary because it should be common sense. Since masks were politicized by our lame duck President we have a nation where many don’t believe wearing a mask is necessary and in turn puts others in harms way.
Spot says
Percy’s mother…Many of us DO have the sense to protect others and ourselves by wearing masks. It is the rest of the irresponsible covidiots who need a mandate from someone in authority in order to even possibly comply. I expect Gov. DeSantis to make the correct decisions for the well being of Floridians, but so far he hasn’t.
Jp says
Fun fact. If I wear my mask and morons who listen to Trump and Desantis don’t, then those idiots are protected from me but I’m not protected from them.
Mike Cocchiola says
And this morning on FM 104.5, a conservative talk show out of Jacksonville, the host bragged about how brave DeSantis was to open the state and how right he was because Florida’s COVID-19 rate has “plummetted”.
This is the fatal nonsense the right-wing feeds on daily and they are endangering people across this nation. It’s not enough for me or you to wear a mask and socially distance ourselves. We all have to do it to help stop the person-to-person spread of this virus. But I suppose that first amendment rights Trump medical science. And we sure don’t want to be accused of waging a medical science war on Christmas. Oh, wait… Tucker Carlson has said just that. We – the vast majority of Americans – are using the coronavirus as an excuse to kill Christmas. The madness.. it hurts!
concerned citizen says
Florida newspaper investigation finds state government misled public on Covid as cases rose
Governor Ron DeSantis and his administration ‘suppressed facts’ and ‘dispensed dangerous misinformation’, according to paper
Florida Governor Ron DeSantis holds a press conference on 30 November 2020.
Florida Governor Ron DeSantis holds a press conference on 30 November 2020. Photograph: Ricardo Ramirez Buxeda/AP
Guardian staff
Fri 4 Dec 2020 08.07 EST
2,730
Florida this week became the third US state to record a million coronavirus cases and yet the public there has been misled by state leadership about the extent and dangers of the pandemic, especially in the run-up to the presidential election, an investigation has concluded.
Governor Ron DeSantis’s administration has been engaged in a pattern of spin and concealment about Covid-19 amid the gravest health threat the state has ever faced, according to a South Florida Sun Sentinel investigation.
Florida’s ‘mini-Trump’ Ron DeSantis under growing pressure as Covid-19 cases surge
Read more
According to the newspaper, Republican DeSantis influenced a state administration that “suppressed unfavorable facts, dispensed dangerous misinformation, dismissed public health professionals, and promoted the views of scientific dissenters” who supported the governor’s ambivalent approach to the disease.
DeSantis declined to be interviewed, the Sun Sentinel said, but it noted he told Fox News’ Tucker Carlson Tonight earlier this week that the media’s criticism of his approach was “all political”.
The investigation found that the Florida department of health’s county-level spokespeople stopped issuing public statements about Covid-19 between September and the 3 November election.
And earlier on in the pandemic state leaders did not release details about the earliest cases in Florida and denied the virus was spreading person to person, despite the fact that coronavirus is highly contagious.
[The rest of the story here.]
concerned citizen says
Governor Ron DeSantis’s administration has been engaged in a pattern of spin and concealment about Covid-19 amid the gravest health threat the state has ever faced, according to a South Florida Sun Sentinel investigation.
palmcoaster says
Meanwhile one of their idiotic attorneys Giuliani in hospital with Covid. well deserved. Too bad that probably was also a good spreader before confined. Imagine what a Christmas for over a quarter million Americans dead and for their grieving families! We kindly declined going to a gathering outdoors and distancing with 2 other couple friends welcoming them to PC a while ago and guess what, one couple now has covid…they are younger and hopefully surviving, at our age we would not, so glad we declined. We have these killer nocking at our doors and people still refuse to take precautions to satisfy Trump, how ignorant is that.
Tim Mcauliffe says
But wait, there’s more. The former data chief in Florida Rebekah Jones, had her home invaded by Florida Police this morning. Her statement
“At 8:30 am this morning, state police came into my house and took all my hardware and tech. They were serving a warrant on my computer after DOH filed a complaint. They pointed a gun in my face. They pointed guns at my kids.
Ms Jones was fired for refusing to fudge data as Governor “Death Santis” demanded.