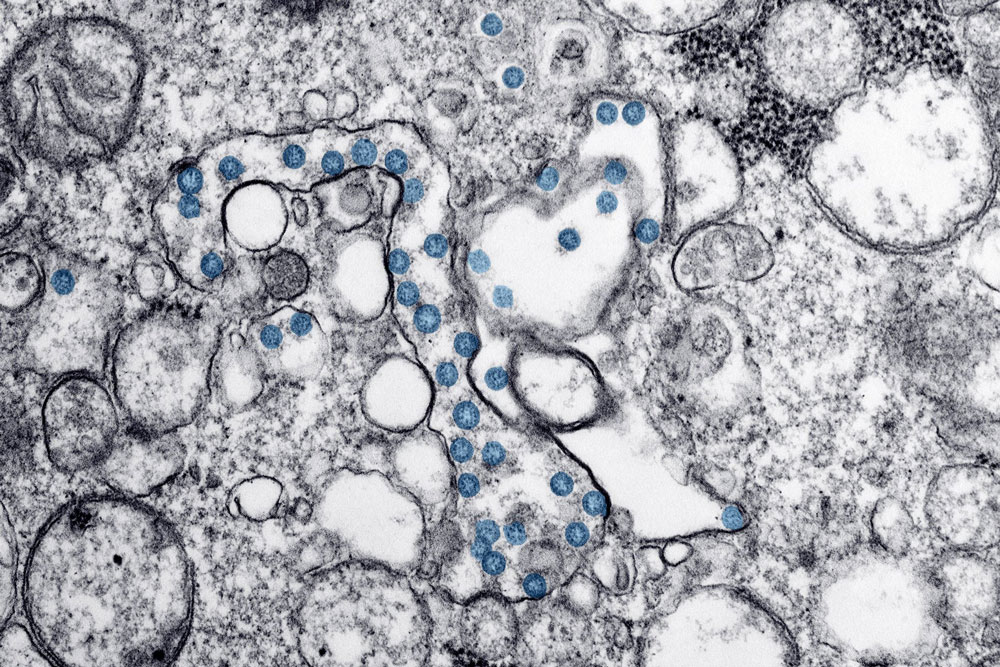
Coronavirus testing capacity will expand next week in Flagler County and across Florida, with capacity for some 625,000 tests available starting Monday, the Flagler Department of Health’s Bob Snyder said on a day roiled by hourly fallout from the virus’ effects locally and across the globe.
“We are going to get to a point where our community is going to have to make some decisions regarding schools,” Snyder had said on the radio just this morning. By late afternoon, the state Department of Education had ordered schools closed at least until March 30. Postponements and cancellations were affecting courts, cultural and social organizations, while the Flagler Chamber of Commerce was switching to remote informational sessions that had previously been scheduled in person.
But a lot remains uncertain about the extent of the virus’ effects locally, how many people it will affect and whether current measures will be enough to stave off a major local outbreak. What is near certain is that the low numbers of Floridians currently testing positive, and the a=bsence of any positives in Flagler, will change rapidly.
Next week, Quest will have the ability of testing 20,000 samples a day in a Tampa lab, Snyder said. “So we’re going to see a huge change when that happens,” he said. “Many more individuals will come out with a positive test result,” because 80 percent have only mild symptoms that can be confused with less serious ailments. “So things are going to change drastically in terms of numbers.”
“That is for nationwide and Florida,” Snyder specified.

(© FlaglerLive)
That still leaves 10 percent of carriers of a virus whose capacities of transmission and potency are still not fully understood.
“This is kind of a moving target because they have sketchy data from a few different places, it’s not complete yet,” Dr. Stephen Bickel, the Florida Department of Health’s medical director, said. And since the virus has an incubation period of up to 14 days for most, with the first symptoms presenting on average at the fifth or sixth day, “there’s no question there’s a risk” of spread, Bickel said, from infected individuals who are walking around without yet showing even mild symptoms.
While there has yet to be a coronavirus case in Flagler, that is more likely due to the dearth of testing–not to the lack of actual cases.
Three factors have Bickel worried: First, the virus “is capable of explosive growth in a population,” with a high contagion rate. Second, “it’s capable of making people pretty darn sick, especially elderly, so it has the potential to overwhelm our healthcare system. That’s what we’re hearing from Italy,” one of the better systems in the world. “The fatality rate is pretty substantial.” Third, surveillance is not easy–meaning that tracing individuals who have it and differentiating them from those who don’t, in the early stages of incubation, is guesswork until symptoms appear–and are diagnosed. “It makes it very hard to contain it,” Bickel said.
“We don’t know what’s going to happen with the virus,” Dr. Timothy Hendricks, Chief Medical Officer for AdventHealth’s CentraCare network, said on Free For All this morning. “We don’t know if it’s going to be widespread through our community, we don’t know what the eventuality is for the need for hospital beds and ICU and ventilators, that type of thing. So our system as a whole, including the AdventHealth Flagler, we are looking at making sure we’re prepared for that surge of patients, and we’ve got the advantage of time now. Italy did not have the advantage of time. They quadrupled their number of cases in a matter of a couple of weeks and put a tremendous strain on their medical system there. We’re looking at examples from even hospitals in Washington State that are dealing with their localized outbreak and how they best manage that and taking those lessons and applying them to our system.”
“We don’t know what’s going to happen with the virus.”
He said there are three different stages in an outbreak: containment–the stage we’re in now, which buys time for the possibility of a widespread outbreak. Mitigation is next, where sick patients are kept as mucha s possible at home and away from the public. “And then the final stage is that surge where we just have too many people coming into the hospital at once. So you’ll hear the term flattening the curve. Epidemiologists love this thing.” He said the spike is reduced through early identification and containment of people “who might have the virus.”
The question is whether sufficient containment measures were in place before the virus has had a chance to migrate forcefully.
Meanwhile, the state Department of Health continues to severely limit the information it is disseminating about the pandemic’s effects in the state and in counties, from the number of tests actually performed to the more precise location and information about patients affected.
The Department of Health is not disclosing how many tests have been carried out in Flagler, and disclosing only that it has 221 pending tests across the state, and 478 negative test results. That suggests the state and counties are conducting very few tests, and thereby undercounting actual cases.
The low number of tests has been driven by the lack of testing kits. Triaging has focused on individuals showing symptoms, Snyder said.
Private physicians have the ability to collect the swabbed specimens, then send the specimens to private laboratories such as LabCorp and Quest for coronavirus testing. Those private labs may soon take the lead in processing the tests, ahead of the state’s own labs in Tampa, Jacksonville and Miami, which have a much more limited capacity to process test–about 150 tests a day, according to Snyder.
For that reason, Snyder said the absence of cases in Flagler is “an illusion” that will soon be dispelled, a caution underscored by Flagler Emergency Management Chief Jonathan Lord.

(© FlaglerLive)
By Friday, the world had recorded 144,000 coronavirus cases, half of whom had recovered. But 5,395 people had died–a staggering 3.7 percent rate. Most of the recoveries are in China, Italy and Iran, the top three hardest-hit countries so far. The United States passed the 2,000-case mark Friday, with 41 deaths, though more than 1,900 cases are still active, with just 31 considered recovered. Cases in Florida jumped to 45, according to the Department of Health–but again, that’s based on a limited number of tests.
Volusia recorded its third case on Thursday, a 70-year-old man who, according to the Department of Health, “is a travel related case and is associated with a Nile River Cruise/Tour in Egypt.”
But it’s not as if there’s been a rush on testing locally: “We haven’t had anyone to do that,” Snyder said, referring to the health department facility in Bunnell, which continues to be fully staffed. “The only thing is we run the HIV clinic, so those are individuals that are immuno-suppressed, so we’ve had a couple of those folks that have called. We talked to them on the phone, they didn’t quite meet criteria to be tested. We’ve had no one from the community come to be tested yet.”
Whether to test or not is still at the Department of Health’s discretion. That’s not necessarily the case with private physicians, who are required by law to disclose any positive test result to the health department.
If an individual shows up without symptoms and demands to be tested at the health department, “We are going to talk to the patient,” Snyder said, “reassure them, because we want to know, do you have the clinical symptoms, same thing as the flu, if you don’t have the clinical symptoms, it doesn’t make sense to test that patient.”
“If someone has the clinical symptoms, flu-like symptoms, fever, shortness of breath, a cough,” he continued, “please, contact your primary care physician, because they’ll be able to provide the test through these commercial labs, or contact the health department, or go to an urgent care center or Azalea health.”
According to officials at the Centers for Disease Control and Prevention, who conferred with prevention experts from around the world last month to map out what might happen if coronovirus landed in the United States, the country is in for a grim few months. The CDC had not intended to disclose its analyses. New York Times reported on the CDC’s findings and subsequent independent analyses based on those findings today.
“The C.D.C.’s scenarios were depicted in terms of percentages of the population,” The Times reported. “Translated into absolute numbers by independent experts using simple models of how viruses spread, the worst-case figures would be staggering if no actions were taken to slow transmission. Between 160 million and 214 million people in the United States could be infected over the course of the epidemic, according to one projection. That could last months or even over a year, with infections concentrated in shorter periods, staggered across time in different communities, experts said. As many as 200,000 to 1.7 million people could die. And, the calculations based on the C.D.C.’s scenarios suggested, 2.4 million to 21 million people in the United States could require hospitalization, potentially crushing the nation’s medical system, which has only about 925,000 staffed hospital beds. Fewer than a tenth of those are for people who are critically ill.”
The paper noted that the assumptions are mitigated by containment measures governments, schools, businesses and others are taking to slow the virus.



























ASF says
I visited two different Publix supermarkets, one in Palm Coast and one in Flagler Beach, on two consecutive days. Both had run completely out of sanitizing wipes with which the public could wipe down the shopping carts. This is a major problem. When I tried to contact the Publix corporate management, local Heath department and Florida Health Department, I got nowhere. When I tried to use the email address for the COVID website on Florida Health Department–[email protected], it didn’t even work. I kept getting email notifications back saying that my email could go through at the email address provided.
ASF says
..excuse me–“email notifications back saying that my email could NOT go through at the email address provided.”
Cynthia says
He says to “ contact your primary health care provider or go to an urgent health care center.” What? He’s advising Flagler Co. residents to go sit in some urgent care wait room thereby assuring that every person waiting to be seen is exposed also exposing the staff? Are we supposed to waltz in there announcing we have flu- like symptoms? The receptionist would need to be wearing full on PPE to avoid exposure along with everyone else. Call our primary care? Is he/she going to send us to Quest? What if they’re closed for the day?! Can someone please explain how testing will actually go down if and when we need it? Be specific sir.
Steve Ward says
SO I am going to bring it. After a month plus of Politicizing the Corona HOAX that will Miraculously dissappear one day ,that the Media and Other Politicians brought their opinions out to the forefront in fashion , the Orangeman blowhard addicted to what he feels is important, himself, has come undone. His failure as a leader can only be amplified by the extent of which our lives have changed under the auspices of a deranged conman unqualified to lead the not so free World as we know it. Failure, fraud, narcissism, contempt, greed at the highest level.Hows your Economy now dimwits. Vote accordingly.
PS WE told ya so……..
OnceagainBS says
Oh please! This virus is being blown out of proportion by the press and it is nothing but an attempt to tank the economy in order to blame Trump! It’s y’alls last ditch effort to prevent him from being re-elected! The press are liberal loons and will do anything to help their cronies. This virus can be killed with over the counter wipes for Gods sake! Stop bashing and pointing fingers and wash your hands! You people, I swear!! Yeah let’s hope they vote accordingly cause otherwise we will be led either by a raging Socialist or a raging dementia inflicted liberal criminal!